
CALIFORNIA
HIV/AIDS POLICY
RESEARCH CENTERS
PrEP Cost Analysis
for Covered California
Health Plans
November 2016
AUTHORS
AJ King, MPH
Craig A. Pulsipher, MPP, MSW
Ian W. Holloway, MSW, MPH, PhD
FUNDER
This study was funded by the California HIV/AIDS Research Program (Grant Number RP15–LA–007).
ACKNOWLEDGMENTS
This study was conducted by the California HIV/AIDS Policy Research Center at UCLA/APLA Health, through a generous
grant from the University of California HIV/AIDS Research Program. Additional support was provided by the Center for HIV
Identification, Prevention, and Treatment Services NIMH grant P30MH58107. We thank Jennifer Gildner and Sean Beougher
for their assistance with fact checking and copyediting. We also wish to thank Sneha Patil from the San Francisco Department
of Public Health, for her valuable input.
ABOUT THE CALIFORNIA HIV/AIDS RESEARCH PROGRAM
The California HIV/AIDS Research Program fosters outstanding and innovative research that responds to
the needs of all people of California, especially those who are often under served, by accelerating progress
in prevention, education, care, treatment, and a cure for HIV/AIDS. The California HIV/AIDS Research
Program supports two Collaborative HIV/AIDS Policy Research Centers, for research and policy analysis
that addresses critical issues related to HIV/AIDS care and prevention in California. These centers include
the University of California, Los Angeles; APLA Health; Los Angeles LGBT Center; University of California,
San Francisco; San Francisco AIDS Foundation; and Project Inform.
King, AJ, Pulsipher CA, Holloway IW. PrEP Cost Analysis for Covered California Health Plans. November 2016.
Introduction
Open enrollment for Covered California, the State’s health
insurance marketplace, begins November 1, 2016. Before
enrolling, there are important things that you should consider
if you’re HIV-negative and interested in accessing HIV pre-
exposure prophylaxis (PrEP). The purpose of this document
is to help you better understand how much you can expect to
pay for PrEP under various Covered California health plans,
as costs to access PrEP vary by income, area of residence,
and other factors.
About PrEP
PrEP is an HIV prevention strategy in which HIV-negative
individuals take a daily medication to reduce their risk of
becoming infected. Currently, the only drug approved by
the Food and Drug Administration to be used for PrEP is
Truvada
®
. People who take PrEP are usually required to see
their healthcare provider for routine testing and follow-up
care. Specifically, according to Clinical Guidelines from the
Centers for Disease Control and Prevention, once PrEP is
initiated, patients should return for follow-up approximately
every 3 months. Not all doctors are familiar with PrEP and
some may resist prescribing it. If you’re interested in PrEP, it’s
important to choose a Covered California plan that ensures
you can find a doctor who will prescribe it. Before you make
any final decisions, be sure that the primary care doctor you
are considering takes the plan you want and is willing to
prescribe PrEP. A list of doctors with experience providing
PrEP can be found at: www.pleaseprepme.org. A flow chart
offering step-by-step instructions for acquiring PrEP can be
found at www.projectinform.org/pdf/PrEP_Flow_Chart.pdf.
More information about PrEP, including effectiveness and
side effects, can be found at www.prepfacts.org.
Overview of Covered California
The Patient Protection and Affordable Care Act (ACA)
PrEP Cost Analysis
for Covered California
Health Plans
enables individuals and small businesses to purchase health
insurance at federally subsidized rates via statewide health
insurance exchanges like Covered California. Under the
ACA, most individuals who are U.S. citizens, U.S. nationals,
or lawfully present immigrants are required to have health
coverage (there is a tax penalty for those who do not have
health coverage and do not qualify for an exemption). All
eligible Californians can sign up during the annual open-
enrollment period from November 1, 2016 to January 31,
2017. Many others may be eligible to sign up at any time
during the year due to a life-changing event, such as getting
married, having a child, or moving. Medi-Cal enrollment for
those with incomes less than 138% of the federal poverty
level (FPL) ($16,394 for individuals in 2017) is year-round
and also accessible via the Covered California website
[www.coveredca.com].
Health Insurance Plans and Pricing Regions
There are 11 health insurance plans available via
Covered California in 2017:
1. Anthem Blue Cross of California
2. Blue Shield of California
3. Chinese Community Health Plan
4. Health Net
5. Kaiser Permanente
6. L.A. Care Health Plan
7. Molina Healthcare
8. Oscar Health Plan of California
9. Sharp Health Plan
10. Valley Health Plan
11. Western Health Advantage
Under Covered California, the state is comprised of 19
different regions—each with different pricing and health
insurance options, as depicted in Figure 1.
Nearly all Covered California consumers have at least three
health insurance companies to choose from in their region

4
Figure 1: Covered California Pricing Regions*
respect to which type or types of insurance they provide.
• HMOs are “managed care” and assign a Primary Care
Physician (PCP) to oversee your care. HMOs usually
require members to get a referral from their PCP to see
specialists and HMOs only cover visits to doctors and
hospitals within their plan’s network.
• PPOs are more flexible when choosing doctors and
specialists. PPOs cover doctor visits inside and outside
their networks. However, you pay a higher cost for out-of-
network care.
• EPOs are similar to PPOs because members may not
need a referral to see a specialist. However, EPOs do not
cover visits to doctors outside the plan’s network. Their
network is “exclusive.”
1
Kaiser and Health Net only cover part of the region
2
Molina Healthcare only covers part of the region
and in some regions consumers have as many as seven. For
example, if you reside in San Francisco, Pricing Region 4, you
can choose from Anthem, Blue Shield, Chinese Community
Health Plan (CCHP), Kaiser Permanente, Health Net, or
Oscar. In Fresno, Pricing Region 11, you can choose from
Anthem, Blue Shield, Kaiser Permanente, or Health Net.
1
Los
Angeles County is divided into two pricing regions: 15 and
16. In Pricing Region 16, you can choose from Anthem, Blue
Shield, Kaiser Permanente, Health Net, LA Care, Oscar, or
Molina Healthcare.
2
There are also three different types of
insurance plans: health maintenance organizations (HMOs),
preferred provider organizations (PPOs), and exclusive
provider organizations (EPOs). Plans vary by region with
1. Northern counties
2. North Bay Area
3. Greater Sacramento
4. San Francisco County
5. Contra Costa County
6. Alameda County
7. Santa Clara County
8. San Mateo County
9. Santa Cruz, San Benito,
Monterey
10. Central Valley
11. Fresno, Kings, Madera
Counties
12. Central Coast
13. Eastern Counties
14. Kern County
15. Los Angeles County
(partial)
16. Los Angeles County
(partial)
17. Inland Empire
18. Orange County
19. San Diego County
* Portions of this section were
drawn directly from the Covered
California website [coveredca.org]
5
The Metal-Category System
Covered California health insurance plans are sold in four
levels of coverage or metal categories: Bronze, Silver,
Gold, and Platinum. As the metal category increases in
value (from Bronze to Platinum), so does the percentage
of medical expenses that a health insurance plan covers
relative to what you are expected to pay in copays and
deductibles. Typically, Platinum plans cover 90% of health
care costs, while you pay 10%; Gold plans cover 80%,
while you pay 20%; Silver plans cover 70%, while you
pay 30%; and Bronze plans cover 60%, while you pay
40%. Plans in higher metal categories have higher monthly
premiums, but when you need medical care you pay less.
You can choose to pay a lower monthly premium, but when
you need medical care you pay more. When deciding
which level of coverage best meets your health needs and
budget, note: If you are interested in accessing PrEP,
Bronze plans should generally be avoided. Despite
their low premiums, they have high deductibles and out-
of-pocket costs that are likely to make accessing some
medications and benefits unaffordable. It's very important,
however, to consider both out-of-pocket costs and monthly
premiums before you select a health plan.
Drug Formularies and Tiers
Each health insurance company has a list of covered
medications, known as a drug formulary. It is important
to remember that a plan’s drug formulary can change
at any time and the plan will have the most up-to-date
formulary. Drugs on the formulary are grouped into four
tiers: generic (Tier 1), preferred (Tier 2), non-preferred
(Tier 3), or specialty (Tier 4). On Covered California you
will be charged no more than $250 per month for one 30-
day supply of a Tier 4, specialty drug for Silver, Gold, and
Platinum plans and no more than $500 per 30-day supply
for Bronze plans. Drugs in lower tiers will have lower costs.
Truvada
®
is currently covered by all Covered California
health plans and is listed as a Tier 2, preferred drug.
Standard Benefits
All health insurance plans sold through Covered California
have standard benefits, including coverage for prescription
drugs, doctor visits, hospitalizations, labs, and mental
health and substance abuse services. Differences in
these standard benefits help consumers compare health
insurance options. It is important to review each plan’s
price, provider network, “Summary of Benefits and
Coverage,” as well as more detailed coverage descriptions,
to find the plan that best suits your needs.
Overview of Costs Associated with Healthcare
There are two cost categories related to having health
insurance and accessing care: monthly premiums (minus
premium assistance, if applicable); and “out of pocket”
costs (minus any cost-sharing subsidies, if applicable).
Monthly Premiums and Premium Assistance
Monthly premiums are the price you pay for having health
insurance, regardless of whether you use it. If your income
is less than or equal to 400% FPL, or $47,520 for a
single person, you may qualify for help paying for your
health insurance premium, regardless of the metal level
you choose. This is known as premium assistance or the
federal government’s “advance premium tax credit.” You
can choose to receive this assistance in one of two ways:
1) as an advance each month, which lowers your monthly
payments, or 2) at the end of the year when you complete
your taxes. The amount you pay in monthly premiums will
vary depending on:
• your age (the older you are, the more expensive health
insurance is);
• your region (typically, if you live in Northern California
you will pay more for health insurance than if you live in
Southern California);
• your income (given that you can get premium
assistance if your income is less than or equal to 400%
FPL, as described above);
• the metal level you choose (you will pay the highest
premiums for Platinum level, followed by Gold, then
Silver, then Bronze).
Covered California recently announced average premium
increases of 13.2 percent for 2017, so it is very important
for consumers to shop to find a plan that best meets their
health needs and budget.
Out-of-Pocket Costs and Cost-Sharing Subsidies
Out-of-pocket costs include an annual deductible, if
applicable, and copays or coinsurance for medications,
lab tests, doctor visits, and hospital stays. If your income
is less than or equal to 250% FPL, or $29,700 for a
single person, you may qualify for cost-sharing subsidies,
which reduce your out-of-pocket costs including copays,
coinsurance and deductibles. They may also reduce your
out-of-pocket maximum. Cost-sharing subsidies are
only available if you select a Silver plan – known as
Enhanced Silver plan. There are three categories of
Enhanced Silver – Silver 73, Silver 87, Silver 94.
For single households, if you make:
• between 139-150% FPL ($16,395 - $17,820), you can
6
qualify for a Silver 94 plan
• between 151-200% FPL ($17,821 - $23,760), you can
qualify for a Silver 87 plan
• between 201-250% FPL ($23,761 - $29,700), you can
qualify for a Silver 73 plan
Drug deductibles and copays are lower for the Silver 94,
87, and 73 than the Silver 70 (basic Silver plan without
enhancements) because costs are subsidized for lower
income individuals to make the plan affordable based on
income.
Out-of-Pocket Maximum
The out-of-pocket maximum is the most you would have
to pay for medical expenses during the year (not including
your monthly premiums). Keep in mind that out-of-pocket
maximums differ depending on your income and which
metal level you select. Deductibles, copays and coinsurance
count toward your out-of-pocket maximum unless they are
considered “out of network” or “not covered.” In most cases,
once you reach your out-of-pocket maximum, your insurance
will cover 100% of the costs they consider medically
necessary. It’s important to understand what out-of- pocket
costs will count toward your out-of-pocket maximum before
signing up for a new health plan.
To summarize, the amount you pay in “out-of-pocket” costs (in
addition to your monthly premium) will vary depending on:
• the amount and type of health services and prescription
medication you access;
• your income (you are eligible for cost sharing subsidies if
your income is between 138% -250% FPL);
• the metal level you choose (highest out-of-pocket costs
for Bronze level);
• your annual deductible;
• your out-of-pocket maximum.
Determining PrEP Costs
The costs associated with taking PrEP include:
1. the cost of medication (Truvada
®
);
2. the cost of doctor visits;
3. the cost of laboratory tests your doctor orders;
4. the cost of health insurance (i.e., your monthly premiums).
Estimating the cost of Truvada
®
Without insurance, Truvada
®
costs approximately $1,250
monthly or $15,000 annually. However, under Covered
California plans, the cost you pay will be much less and
depends on your plan’s drug formulary and the metal
level you choose. Across all Covered California plans,
Truvada
®
is listed as a Tier 2 or preferred drug. Gilead, the
company that manufactures Truvada
®
, offers a copay card
to help cover the cost of the medication for those who
have insurance – up to $3,600 a year. Table 1 depicts the
annual cost of Truvada
®
by metal level with and without
the Gilead copay card. These costs were calculated
using information from Covered California’s 2017 Patient-
Centered Benefit Designs and Medical Cost Shares. A
12-month supply of Truvada
®
ranges from $120 - $6,000
without the Gilead copay card, and from $0 - $2,400 with
the Gilead copay card, depending on the metal level you
choose. Information about the copay program can be found
at www.gileadcopay.com. You may also be able to obtain
financial assistance from the Patient Access Network at
www.panfoundation.org/fundingapplication/welcome.php
or the Patient Advocate Foundation at www.copays.org/
diseases/hiv-aids-and-prevention.
California’s PrEP Financial Assistance Program
In spring 2017, the California Department of Public Health,
Office of AIDS will launch a PrEP financial assistance
program. The program will cover PrEP-related out-of-
pocket costs (e.g., copays for medication, doctor visits,
and laboratory tests) for qualified individuals with annual
incomes below 500% FPL.
Estimating additional out-of-pocket costs
and monthly premiums
Additional out-of-pocket costs for PrEP, including doctor
visits, laboratory tests, as well as deductibles and out-
of-pocket maximums, are summarized by metal level in
Table 2. Cost estimates include five doctor visits and five
labs during the first year of PrEP initiation to account
for the initial visit, a one-month follow-up visit, and then
three additional follow-up visits every three months for the
duration of the year. Additionally, out-of-pocket maximums
may vary from plan to plan with respect to whether they
include deductibles. For our cost estimations, we assume
that deductibles count towards out-of-pocket maximums.
In our calculations, we assume a primary care visit costs
$200. Out-of-pocket costs may be more if you are required
to see a specialist.
As described above, monthly premiums vary significantly
based on a number of factors. To illustrate this point, Table
3 lists the monthly premiums for health plans available in
Los Angeles, San Francisco, and Fresno, by metal level, for
different ages. These premiums don’t include all options
under each plan (e.g. EPOs and PPOs were not included if
an HMO was also available). These premiums also do not
include any premium assistance or tax savings, given they
7
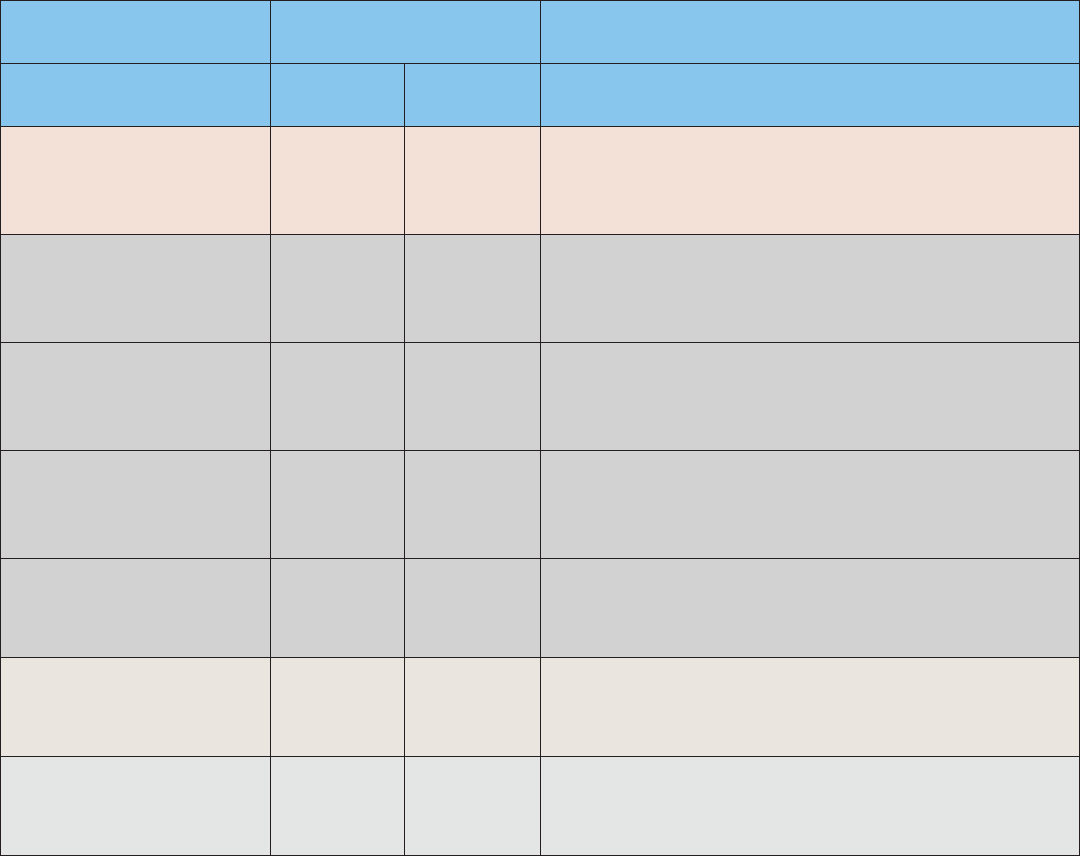
Covered California
Metal Levels
Truvada
®
Cost How Cost was Calculated
Without Gilead
co-pay card
With Gilead
co-pay card
Bronze $6,000 $2,400
$500 pharmacy deductible
Full cost up to $500 after drug deductible is met:
1st month: $500 (deductible met)
2nd – 12th month: $500/month = $5,500
Silver $855 $0
$250 pharmacy deductible
$55 copay/month:
1st month: $250 (deductible met)
2nd – 12th month: $55/month = $605
Silver - Enhanced 73* $800 $0
$250 pharmacy deductible
$50 copay/month:
1st month: $250 (deductible met)
2nd – 12th month: $50/month = $550
Silver - Enhanced 87* $270 $0
$50 pharmacy deductible
$20 copay/month:
1st month: $50 (deductible is met)
2nd – 12th month: $20/month = $220
Silver - Enhanced 94* $120 $0
No deductible
$10 copay/month:
1st – 12th month: $10/month = $120
Gold $660 $0
No deductible
$55 copay/month:
1st – 12th month: $55/month = $660
Platinum $180 $0
No deductible
$15 copay/month:
1st – 12th month: $15/month = $180
*These metal levels have the cost-sharing subsidies built in.
were calculated for individuals with incomes above 400%
FPL or $47,520 for a single person. Finally, Tables 4, 5,
and 6 estimate the total costs (out-of-pocket costs and
monthly premiums) associated with accessing PrEP via
Covered California for fictitious individuals of different ages
and incomes living in different regions of California. Table 7
demonstrates how those costs were calculated.
Selecting the best Covered California health plan to meet
your overall healthcare needs can be challenging. Certified
Enrollment Counselors and Insurance Agents, as well
as Covered California Call Center representatives, are
available to answer questions about financial assistance
and can help you compare plans. You can find free,
confidential, in-person help at http://www.coveredca.com/
get-help/local/.
Table 1: Summary of Annual Truvada
®
Costs by Metal Level

8
Covered California
2017 Metal Levels
Estimated Annual Cost
of Truvada
®
Cost of Care Accessed
(5 doctor visits and 5 labs
per year)
Estimated Annual
OOP Costs
Bronze
Max OOP
1
: $6,800
$6,000
(with Gilead copay card: $2400)
Primary Care
2
Visits:
$75 for first 3 visits and full
cost for 4th and 5th visits until
deductible is met = $225 +
(~$200 x 2) = $625
6000
625
+200
$6,825
$6,825
OOP MAX = $6,800
($3,200 with Gilead copay card)
Laboratory Tests:
$40 x 5 per year = $200
Silver 70
Available for individuals with
income above $29,701
(≥251% FPL)
Max OPP: $6,800
$855
(with Gilead copay card: $0)
Primary Care Visits:
$35 x 5 = $175
855
175
+175
$1,205
($350 with Gilead copay card)
Laboratory Tests:
$35 x 5 per year = $175
Silver 73
For individuals with income
$23,761-$29,700
(>200% to ≤250% FPL)
Max OOP: $5,700
$800
(with Gilead copay card: $0)
Primary Care Visits:
$30 x 5 = $150
800
150
+175
$1,125
($325 with Gilead copay card)
Laboratory Tests:
$35 x 5 per year = $175
Silver 87
For individuals with income
$17,821-$23,760
(>150% to ≤200% FPL)
Max OOP: $2,350
$270
(with Gilead copay card: $0)
Primary Care Visits:
$10 x 5 = $50
270
50
+75
$395
($125 with Gilead copay card)
Laboratory Tests:
$15 x 5 per year = $75
Silver 94
For individuals with incomes up
to $17,820 (150% FPL)
Max OPP: $2,350
$120
(with Gilead copay card: $0)
Primary Care Visits:
$5 x 5 = $25
120
25
+40
$185
($65 with Gilead copay card)
Laboratory Tests:
$8 x 5 per year = $40
Table 2: Summary of Estimated Out-of-Pocket (OOP) Costs for PrEP by Metal Level
1
Max OOP refers to the maximum amount you’ll have to pay during a policy period for health services (usually a year).
Once you reach your Max OPP your plan begins to pay 100 percent of the covered services.
2
Specialist visits may be slightly higher

9
Covered California
2017 Metal Levels
Estimated Annual Cost
of Truvada
®
Cost of Care Accessed
(5 doctor visits and 5 labs
per year)
Estimated Annual
OOP Costs
Gold
Max OOP: $6,750
$660
(with Gilead copay card: $0)
Primary Care Visits:
$30 x 5 = $150
660
150
+175
$985
($325 with Gilead copay card)
Laboratory Tests:
$35 x 5 per year = $175
Platinum
Max OOP: $4,000
$180
(with Gilead copay card: $0)
Primary Care Visits:
$15 x 5 = $75
180
75
+100
$355
($175 with Gilead copay card)
Laboratory Tests:
$20 x 5 per year = $100
Range Across Plans
$120-$6,000
($0-$2,400 with Gilead
copay card)
$185-$6,800
($65 - $3,200 with
Gilead copay card)
Table 2: Summary of Estimated Out-of-Pocket (OOP) Costs for PrEP by Metal Level (cont’d.)

10
CCHP Oscar Kaiser Blue Shield
SF SF LA SF LA Fresno SF LA Fresno
Bronze
Age 20 $156 $185 $127 $160 $121 $123 $204 $161 $137
Age 30 $279 $330 $227 $286 $216 $221 $354 $288 $245
Age 40 $314 $372 $256 $322 $243 $248 $411 $324 $276
Age 50 $438 $519 $357 $450 $340 $347 $575 $453 $385
Silver 70
Age 20 $202 $240 $165 $221 $167 $170 $247 $178 $161
Age 30 $361 $429 $295 $394 $298 $304 $441 $318 $288
Age 40 $407 $483 $332 $444 $335 $342 $497 $358 $324
Age 50 $569 $675 $465 $620 $469 $479 $694 $501 $453
Gold
Age 20 $250 $278 $191 $256 $193 $197 $299 $216 $200
Age 30 $445 $497 $342 $457 $345 $352 $535 $386 $358
Age 40 $502 $560 $385 $514 $389 $397 $602 $434 $403
Age 50 $701 $782 $538 $719 $453 $555 $842 $607 $563
Platinum
Age 20 $275 $316 $217 $282 $213 $218 $370 $267 $256
Age 30 $491 $565 $389 $504 $381 $389 $661 $477 $458
Age 40 $553 $636 $438 $568 $429 $438 $744 $537 $515
Age 50 $773 $888 $611 $794 $600 $612 $1,040 $750 $720
Table 3: Monthly Premiums for Individuals with incomes above 400% FPL in San Francisco, Los Angeles,
and Fresno

11
Anthem Blue Health Net Molina LA Care
SF LA Fresno SF LA Fresno LA LA
Bronze
Age 20 $190 $147 $125 $203 $154 $167 $100 $120
Age 30 $340 $263 $223 $364 $275 $299 $178 $215
Age 40 $382 $296 $251 $409 $310 $337 $201 $242
Age 50 $534 $414 $351 $572 $433 $470 $280 $338
Silver 70
Age 20 $270 $150 $205 $270 $144 $222 $127 $134
Age 30 $482 $268 $366 $482 $257 $397 $227 $240
Age 40 $543 $302 $412 $543 $289 $447 $256 $270
Age 50 $759 $422 $575 $759 $404 $624 $358 $378
Gold
Age 20 $341 $184 $250 $336 $181 $277 $143 $158
Age 30 $610 $328 $447 $601 $324 $495 $255 $283
Age 40 $686 $370 $504 $677 $364 $557 $287 $319
Age 50 $959 $517 $704 $946 $509 $778 $401 $445
Platinum
Age 20 $406 $221 $301 $397 $201 $327 $165 $184
Age 30 $725 $395 $539 $710 $359 $584 $295 $329
Age 40 $816 $445 $607 $800 $404 $658 $332 $370
Age 50 $1,141 $622 $848 $1,118 $564 $919 $464 $518
Table 3: Estimated monthly premiums for individuals with incomes above 400% FPL in San Francisco,
Los Angeles, and Fresno (cont’d.)

12
Table 4: Estimated costs to access PrEP for a 25 year-old individual with an income of $17,820 (150% FPL)
in Los Angeles
BRONZE
Molina LA Care Health Net Anthem Blue Oscar Kaiser Blue Shield
Monthly
Premium
6
$6
x 12 = $72
$38
x 12 = $456
$92 HSP
x 12 = $1,104
$81 EPO
x 12 = $972
$49 EPO
x 12 = $588
$39
x 12 = $468
$103 PPO
x 12 = $1,236
Doctor Visits 1st 3 @ $75, then full cost (~$200) until deductible is met = $625
Labs $40/per x 5 = $200
Truvada
®
Full cost up to $500/mo. after $500 deductible is met = $6,000
Deductible $6,300 medical/ $500 pharmacy
OOP Max $6,800
TOTAL COST
(w/Gilead
copay card )
$6,872
($3,272)
$7,256
($3,656)
$7,904
($4,304)
$7,772
($4,172)
$7,388
($3,788)
$7,268
($3,668)
$8,036
($4,436)
SILVER 94
Molina LA Care Health Net Anthem Blue Oscar Kaiser Blue Shield
Monthly
Premium
$49
x 12 = $588
$60
x 12 = $720
$75
x 12 = $900
$85 HMO
x 12 = $1,020
or
$178 EPO
x 12 = $2,136
$109
x 12 = $1,308
$111
x 12 = $1,332
$129 HMO
x 12 = $1,548
or
$147 PPO
x 12 = $1,764
Doctor Visits $5/per x 5 = $25
Labs $8/per x 5 = $40
Truvada
®
$10/per x 12 = $120
Deductible $75/$0
OOP Max $2,350
TOTAL COST
(w/Gilead
copay card )
$773
($653)
$905
($785)
$1,085
($965)
$1,205
($1,085)
or
$2,321
($2,201)
$1,493
($1,373)
$1,517
($1,397)
$1,733
($1,613)
or
$1,949
($1,829)
1
Premium reflects a tax credit (i.e. financial assistance)

13
GOLD
Molina LA Care Health Net Anthem Blue Oscar Kaiser Blue Shield
Monthly
Premium
$74
x 12 = $888
$98
x 12 = $1,176
$134
x 12 = $1,608
$138 HMO
x 12 = $1,656
or
$266 EPO
x 12 = $3,192
$151 EPO
x 12 = $1,812
$153
x 12 = $1,836
$189 HMO
x 12 = $2,268
or
$220 PPO
x 12 = $2,640
Doctor Visits $30/per x 5 = $150
Labs $35/per x 5 = $175
Truvada
®
$55 x 12 = $660
Deductible $0/$0
OOP Max $6,750
TOTAL COST
(w/Gilead
copay card )
$1,873
($1,213)
$2,161
($1,501)
$2,593
($1,933)
$2,641
($1,981)
or
$4,177
($3,517)
$2,797
($2,137)
$2,821
($2,161)
$3,253
($2,593)
or
$3,625
($2,965)
PLATINUM
Molina LA Care Health Net Anthem Blue Oscar Kaiser Blue Shield
Monthly
Premium
$109
x 12 = $1,308
$139
x 12 = $1,668
$165
x 12 = $1,980
$198 HMO
x 12 = $2,376
or
$345 EPO
x 12 = $4,140
$192 EPO
x 12 = $2,304
$185
x 12 = $2,220
$270 HMO
x 12 = $3,240
or
$324 PPO
x 12 = $3,888
Doctor Visits $15/per x 5 = $75
Labs $20/per x 5 = $100
Truvada
®
$15 x 12 = $180
Deductible $0/$0
OOP Max $4,000
TOTAL COST
(w/Gilead
copay card )
$1,663
($1,483)
$2,023
($1,843)
$2,335
($2,155)
$2,731
($2,551) or
$4,495
($4,315)
$2,659
($2,479)
$2,575
($2,395)
$3,595
($3,415) or
$4,243
($4,063)
Table 4: Estimated costs to access PrEP for a 25 year-old individual with an income of $17,820 (150% FPL)
in Los Angeles (con’t.)

14
Table 5: Estimated costs to access PrEP for a 40 year-old individual with an income of $29,700 (250% FPL)
in San Francisco
BRONZE
CCHP Health Net Anthem Blue Oscar Kaiser Blue Shield
Monthly
Premium
1
$74
x 12 = $888
$169 EPO
x 12 = $2,028
$142 EPO
x 12 = $1,704
$132 EPO
x 12 = $1,584
$82
x 12 = $984
$171 PPO
x 12 = $2,052
Doctor Visits 1st 3 @ $75, then full cost (~$200) until deductible is met = $625
Labs $40/per x 5 = $200
Truvada
®
Full cost up to $500/mo. after $500 deductible is met = $6,000
Deductible $6,300/$500
OOP Max $6,800
TOTAL COST
(w/Gilead co-
pay card )
$7,688
($4,088)
$8,828
($5,228)
$8,504
($4,904)
$8,384
($4,784)
$ 7,78 4
($4,184)
$8,852
($5,252)
SILVER 73
CCHP Health Net Anthem Blue Oscar Kaiser Blue Shield
Monthly
Premium
$167
x 12 = $2,004
$303 EPO
x 12 = $3,636
$303 EPO
x 12 = $3,636
$243 EPO
x 12 = $2,916
$204
x 12 = $2,448
$257 HMO
x 12 = $3,084
or
$244 PPO
x 12 = $2,928
Doctor Visits $30/per x 5 = $150
Labs $35/per x 5 = $175
Truvada
®
$50/per after deductible = $800
Deductible $2200/$250
OOP Max $5,700
TOTAL COST
(w/Gilead co-
pay card )
$3,129
($2,329)
$4,761
($3,961)
$4,761
($3,961)
$4,041
($3,241)
$3,573
($2,773)
$4,209
($3,409)
or
$4,053
($3,253)
1
Premium reflects a tax credit (i.e. financial asssitance)

15
GOLD 80
CCHP Health Net Anthem Blue Oscar Kaiser Blue Shield
Monthly
Premium
$262
x 12 = $3,144
$437 EPO
x 12 = $5,244
$446 EPO
x 12 = $5,352
$320 EPO
x 12 = $3,840
$274
x 12 = $3,288
$362 HMO
x 12 = $4,344
or
$361 PPO
x 12 = $4,332
Doctor Visits $30/per x 5 = $150
Labs $35/per x 5 = $175
Truvada
®
$55 x 12 = $660
Deductible $0/$0
OOP Max $6750
TOTAL COST
(w/Gilead co-
pay card )
$4,129
($3,469)
$6,229
($5,569)
$6,337
($5,677)
$4,825
($4,165)
$4,273
($3,613)
$5,329
($4,669) or
$5,317
($4,657)
PLATINUM
CCHP Health Net Anthem Blue Oscar Kaiser Blue Shield
Monthly
Premium
$313
x 12 = $3,756
$560 EPO
x 12 = $6,720
$576 EPO
x 12 = $6,912
$396 EPO
x 12 = $4,752
$328
x 12 = $3,936
$504 HMO
x 12 = $6,048
or
$529 PPO
x 12 = $6,348
Doctor Visits $15/per x 5 = $75
Labs $20/per x 5 = $100
Truvada
®
$15 x 12 = $180
Deductible $0/$0
OOP Max $4,000
TOTAL COST
(w/Gilead co-
pay card )
$4,111
($3,931)
$7,075
($6,895)
$7,267
($7,087)
$5,107
($4,927)
$4,291
($4,111)
$6,403
($6,223) or
$6,703
($6,523)
Table 5: Estimated costs to access PrEP for a 40 year-old individual with an income of $29,700 (250% FPL)
in San Francisco (con’t.)

16
Table 6: Estimated costs to access PrEP for a 50 year-old individual with an income of $47,520 (400% FPL)
in Fresno
BRONZE
Health Net Anthem Blue Kaiser Blue Shield
Monthly
Premium
$378
x 12 = $4,536
$258 (PPO)
x 12 = $3,096
$254
x 12 = $3,048
$292 (PPO)
x 12 = $3,504
Doctor Visits 1st 3 @ $75, then full cost (~$200) until deductible is met = $625
Labs $40/per x 5 = $200
Truvada
®
Full cost up to $500/mo. after $500 deductible is met = $6,000
Deductible $6,300/$500
OOP Max $6,800
TOTAL COST
(w/Gilead copay card )
$11,336
($7,736)
$9,896
($6,296)
$9,848
($6,248)
$10,304
($6,704)
SILVER 70
Health Net Anthem Blue Kaiser Blue Shield
Monthly
Premium
$531
x 12 = $6,372
$482
x 12 = $5,784
or
$406 (PPO)
x 12 = $4,872
$386
x 12 = $4,632
$360 (PPO)
x 12 = $4,320
Doctor Visits $35/per x 5 = $175
Labs $35/per x 5 = $175
Truvada
®
$55/per after deductible = $855
Deductible $2,500/$250
OOP Max $6,800
TOTAL COST
(w/Gilead copay card )
$7,577
($6,722)
$6,989
($6,184)
or
$6,077
($5,222)
$5,837
($4,982)
$5,525
($4,670)

17
Table 6: Estimated costs to access PrEP for a 50 year-old individual with an income of $47,520 (400% FPL)
in Fresno (cont'd)
GOLD 80
Health Net Anthem Blue Kaiser Blue Shield
Monthly
Premium
$685
x 12 = $8,220
$611
x 12 = $7,332
or
537 (PPO)
x 12 = $6,444
$462
x 12 = $5,544
$470 (PPO)
x 12 = $5,640
Doctor Visits $30/per x 5 = $150
Labs $35/per x 5 = 175
Truvada
®
$55 x 12 = $660
Deductible $0/$0
OOP Max $6,750
TOTAL COST
(w/Gilead copay card )
$9,205
($8,545)
$8,317
($7,657) or
$7,429
($6,769)
$6,529
($5,869)
$6,625
($5,965)
PLATINUM
Health Net Anthem Blue Kaiser Blue Shield
Monthly
Premium
$826
x 12 = $9,912
$755
x 12 = $9,060
or
$657 (PPO)
x 12 = $7,884
$519
x 12 = $6,228
$627 (PPO)
x 12 = $7,524
Doctor Visits $15/per x 5 = $75
Labs $20/per x 5 = $100
Truvada
®
$15 x 12 = $180
Deductible $0/$0
OOP Max $4,000
TOTAL COST
(w/Gilead copay card )
$10,267
($10,087)
$9,415
($9,235) or
$8,239
($8,059)
$6,583
($6,403)
$7,879
($7,699)
18
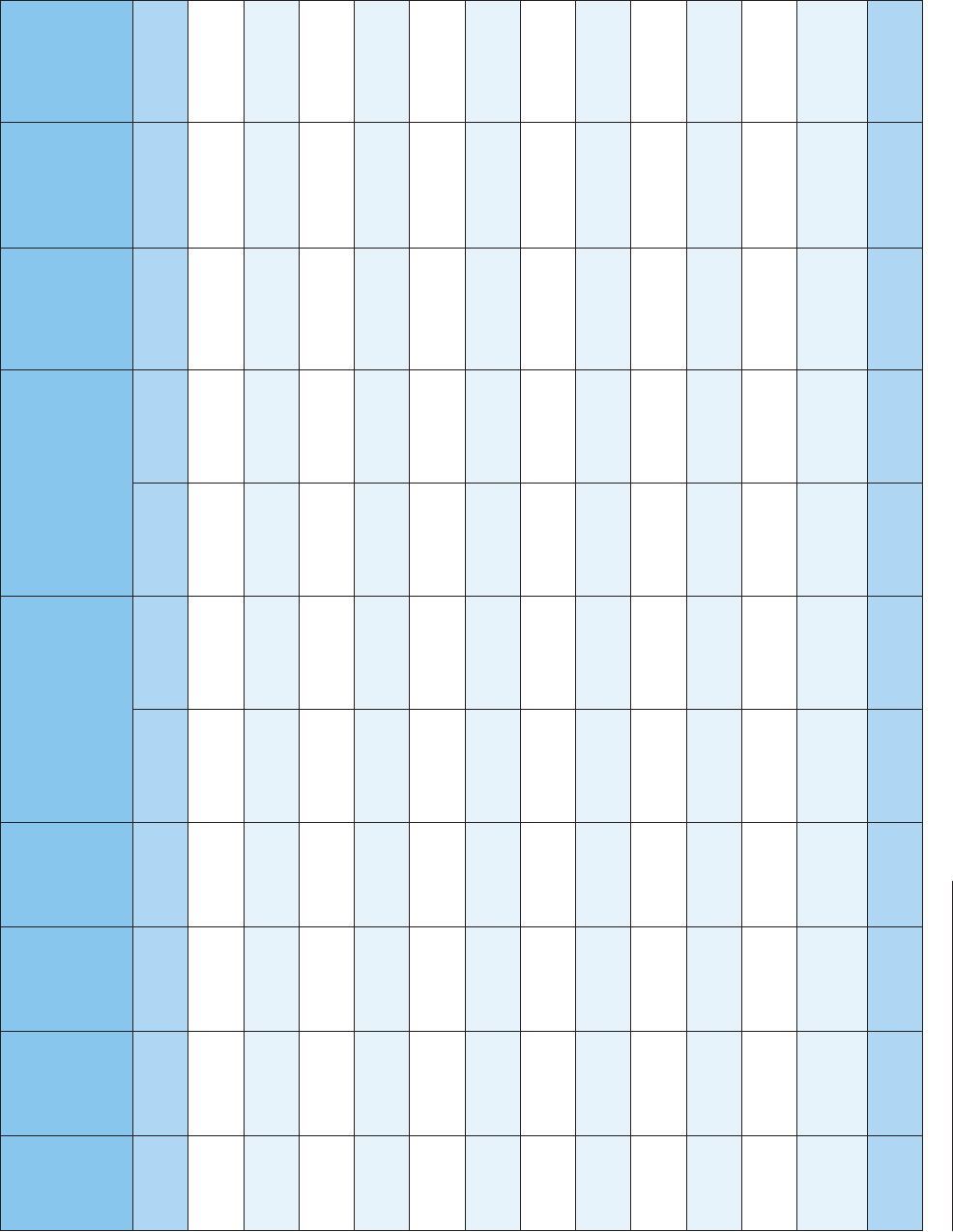
Table 7: Example of Cost Breakdown for Molina Healthcare Bronze Level Plan in Los Angeles
Monthly
Premium
Doctor
Visit
Lab Truvada
®
Total Spent
by Consumer
Cumulative
Total Spent
“OOP”
Amount
Applied
Toward Drug
Deductible/
Mo.
Cumulative
Amount
Applied
Toward Med.
Deductible/
Mo
Without
copay card
With
copay card
Without
copay card
With
copay card
Jan. $6 $75 $40 $500 $200 $621 $321 $615 $500: MET $115
Feb. $6 $75 $40 $500 $200 $621 $321 $1,230 — $230
March $6 — — $500 $200 $506 $206 $1,730 — $230
April $6 — — $500 $200 $506 $206 $2,230 — $230
May $6 $75 $40 $500 $200 $621 $321 $2,845 — $345
June $6 — — $500 $200 $506 $206 $3,345 — $345
July $6 — — $500 $200 $506 $206 $3,845 — $345
August $6 $200 $40 $500 $200 $746 $446 $4,585 — $585
Sept. $6 — — $500 $200 $506 $206 $5,085 — $585
Oct. $6 — — $500 $200 $506 $206 $5,585 — $585
Nov. $6 $200 $40 $500 $200 $746 $446 $6,329 — $825
Dec. $6 — —
$475
+$25*
$171
+$29*
$481 $181
$6,800
OPP MAX
MET
— —
Total $72 $625 $200 $6,000 $2,400 $6,872 $3,272 $6,800 — $825
* Paid for by plan after OOP maximum is reached
Glossary
Premium
The amount you pay every month for your health insurance
plan.
Deductible
The amount you pay before the health plan begins to pay.
Plans can have different deductibles – one for medical costs
like doctor visits or lab work and another one for drugs, or
they can combine the two.
Copay
A fixed amount you pay for services until you reach the out-
of-pocket maximum. For example, you might pay $20 for a
doctor visit and $40 for an x-ray.
Coinsurance
A fixed percentage of the cost of the service that you pay
until you reach your out-of-pocket maximum. For example,
you might pay 30% of the cost of your lab test. Coinsurance
can make it difficult to determine the exact amount of out-
of-pocket cost as it is extremely difficult to find the cost of a
particular service.
Out-of-Pocket Maximum
The most you have to pay for medical expenses during the
year above and beyond your monthly premium. Depending on
your plan, these expenses may include an annual deductible,
co-insurance and co-pays for doctor visits, lab tests, and
prescription drugs. Deductibles, co-pays, and co-insurance
count toward your out-of-pocket maximum unless they are
considered “out of network” or “not covered.” Premiums do
not count. In most cases, once you reach your out-of-pocket
maximum, your insurance will cover 100% of the costs they
consider medically necessary.
Formulary
The set of prescription drugs covered by a health insurance
plan. Drugs on the formulary are grouped into four tiers:
generic (Tier 1), preferred (Tier 2), non-preferred (Tier 3), or
specialty (Tier 4).
References
This report was compiled from information obtained via the
Covered California website (http://www.coveredca.com) and
Project Inform’s “How to choose a health plan in Covered
California” (http://www.projectinform.org/pdf/CCguide.pdf).

20
