
National Aeronautics and Space Administration
Space Faring
The Radiation Challenge
Middle School
Educator Guide
An Interdisciplinary Guide
on Radiation and Human
Space Flight
Educational Product
Grades
Educators
6– 8
EP-2008-08-120-MSFC

i
Space Faring: The Radiation Challenge
Radiation Educator Guide
Middle School Educator Guide
Prepared by:
Jon Rask, M.S., ARC Education Specialist
Wenonah Vercoutere, Ph.D., NASA ARC Subject Matter Expert
Barbara J. Navarro, M.S., NASA ARC Project Manager
Al Krause, MSFC Education Specialist

iii
Space Faring: The Radiation Challenge
Table of Contents
Introduction …………………………………………………………………………………………… v
e Lunar Outpost Scenario
…………………………………………………………………………… v
Radiation
………………………………………………………………………………………………1
Pretest Activities ………………………………………………………………………………… 10
Activity 1: Radiation Exposure on Earth ………………………………………………………… 14
Radiation Damage in Living Organisms
…………………………………………………………… 24
Activity 2: Modeling Radiation Damaged DNA ………………………………………………… 32
Protection from Radiation
…………………………………………………………………………… 42
Activity 3: Space Weather Forecasting …………………………………………………………… 46
Applications to Life on Earth: Radiation as a Tool
…………………………………………………… 56
Glossary
…………………………………………………………………………………………… 61

v
Space Faring: The Radiation Challenge
Introduction
Radiation biology is an interdisciplinary science that examines the biological eects of radiation on living systems. To fully under-
stand the relationship between radiation and biology, and to solve problems in this eld, researchers incorporate fundamentals of
biology, physics, astrophysics, planetary science, and engineering. e Space Faring: e Radiation Challenge educator guide helps
to link these disciplines by providing background, discussion questions, objectives, research questions, and inquiry-based activities
to introduce radiation biology into your middle school science classroom. e suggested activities are hands-on investigations that
encourage the use of science, mathematics, engineering, technology, problem solving, and inquiry skills. e activities provide a
general framework that can be modied based on student needs and classroom resources. is guide is aligned with the National
Science Education Standards of Science as Inquiry, Physical Science, and Life Science, and has been organized into the following
sections and activities:
1. Radiation: Radiation Exposure on Earth
2. Radiation Damage in Living Organisms: Modeling Radiation-Damaged DNA
3. Protection from Radiation: Space Weather Forecasting
4. Applications to Life on Earth: Radiation as a Tool
e major goal of NASA’s Space Radiation Project is to enable human exploration of space without exceeding an acceptable level
of risk from exposure to space radiation (for more information, see ht tp://hacd.jsc.nasa.gov/projects/space_radiation.cfm). Space
radiation is distinct from common terrestrial forms of radiation. Our magnetosphere protects us from signicant exposure to radi-
ation from the sun and from space. Radiation that is emitted from the sun is comprised of uctuating levels of high-energy pro-
tons. Space radiation consists of low levels of heavy charged particles. High-energy protons and charged particles can damage both
shielding materials and biological systems. e amount, or dose, of space radiation is typically low, but the eects are cumulative.
Solar activity uctuates, and so the risk of exposure increases with the amount of time spent in space. erefore there is signicant
concern for long-term human space travel. Possible health risks include cancer, damage to the central nervous system, cataracts,
risk of acute radiation sickness, and hereditary eects. Because there is limited data on human response to space radiation, scien-
tists have developed methods to estimate the risk. is is based on theoretical calculations and biological experimentation. NASA
supports research to analyze biological eects at ground-based research facilities where the space radiation environment can be sim-
ulated. Research performed at these facilities is helping us to understand and reduce the risk for astronauts to develop biological
eects from space radiation, to ensure proper measurement of the doses received by astronauts on the International Space Station
(ISS) and in future spacecraft, and to develop advanced materials that improve radiation shielding for future long-duration space
exploration on the Moon and possibly on Mars.
For over 35 years, NASA has been collecting and monitoring the radiation doses received by all NASA astronauts who have trav-
eled into space as part of the Gemini, Apollo, Skylab, Space Shuttle, Mir, and ISS programs (for more information, see ht tp://srag-
nt.jsc.nasa.gov/). While uncertainties in predicting the nature and magnitude of space radiation biological risks still remain
1
, data
on the amount of space radiation and its composition are becoming more readily available, and research is helping to identify the
biological eects of that radiation.
The Lunar Outpost Scenario
is guide is designed to provide you with information that will be helpful in understanding why radiation research is a crucial
component in the development and planning of long-duration human space exploration. To help inspire students in your classroom,
we suggest that you provide your students with a scenario that encompasses the radiation biology problems involved with human
space exploration of the Moon, including the development of a permanently human-tended lunar outpost, as seen in gure 1
2
.
If such an outpost is to be safely constructed and occupied by people from Earth, we must have a complete understanding of how
the biological limitations of the human body in the space environment will aect its overall design and operation. To successfully
1 Lancet Oncol 2006; 7:431-35
2 ht tp://spaceight.nasa.gov/gallery/images/exploration/lunarexploration/html/s89_26097.html

vi
Space Faring: The Radiation Challenge
grasp the importance of radiation biology, your students will need a solid understanding of why the radiation encountered
in long-duration space exploration is such an enormous challenge to the human body.
A Brief History of Humans on the Moon
It is important to note that the NASA Apollo program was designed to land humans on the Moon and bring them safely back to
Earth; it was not designed to establish a permanent presence on the Moon. e duration of the lunar surface missions were very
short, largely due to the risks of space radiation exposure and the unpredictable nature of the solar weather.
Between 1969 and 1972, six of the seven lunar landing missions (including Apollo 11, 12, 14, 15, 16, and 17) were successful and
enabled 12 astronauts to walk on the Moon. While on the surface, the astronauts carried out a variety of lunar surface experiments
designed to study lunar soil mechanics, meteoroids, seismic activity, heat ow, lunar ranging, magnetic eld distributions, and
solar wind activity. e astronauts also gathered samples and returned to Earth with over 600 pounds of Moon rocks and dust.
Since 1972, no human has returned to the Moon.
e table below shows the amount of time astronauts spent on the surface of the Moon during each lunar landing, and the average
radiation dose they recieved.
Mission Total Duration Lunar Surface Duration Average Radiation Dose*
Apollo 11 08 days, 03 hrs, 13 mins 21 hrs, 38 mins 0.18 rad
Apollo 12 10 days, 4 hrs, 31 mins 31 hrs, 31 mins 0.58 rad
Apollo 14 09 days, 01 min 33 hrs 31 mins 1.14 rad
Apollo 15 10 days, 01 hr, 11 mins 66 hrs, 54 mins 0.30 rad
Apollo 16 11 days, 01 hr 51 mins 71 hrs, 2 mins 0.51 rad
Apollo 17 12 days, 13 hrs, 51 mins 74 hrs, 59 mins 0.55 rad
* Average radiation dose information can be found on the Life Sciences Data Archive at JSC.
3
rough these and robotic missions (ht tp://nssdc.gsfc.nasa.gov/planetary/lunar/apollo_25th.html) including the three Russian
Luna sample return missions, NASA Lunar Prospector (ht tp://lunar.arc.nasa.gov), and the upcoming Lunar Precursor and Robotic
Program (ht tp://lunar.gsfc.nasa.gov), scientists have learned and will continue to learn a great deal about how and when the Moon
was formed, how it may have played an important role in the origin of life here on Earth, and the environment, including radia-
tion, on and below the Moon’s surface.
Figure 1: An artist’s conception of a future Moon base.
3 ht tp://lsda.jsc.nasa.gov/books/apollo/Resize-jpg/ts2c3-2.jpg

vii
Space Faring: The Radiation Challenge
Future Lunar Colonization
Ask your students questions intended to prompt them into thinking about what biological requirements must be met for successful
long-term human exploration of the Moon.
4
Consider what limitations the human body presents in such an endeavor. Start by ask-
ing: “If you had to prepare for future lunar colonization, what would you need and need to know in order to accomplish this task
safely?” To establish a permanently inhabited lunar outpost, your team will need to understand how the space radiation environ-
ment aects living systems.
Exploring the surrounding lunar landscape (see gure 2) and traveling to remote locations on the Moon may also be part of the
activities lunar explorers will perform. Remind your students that there are unknowns about the proposed long-duration exploration
of the Moon. Students will need to understand the hazards of solar and cosmic radiation, their impact on materials and the human
body, the radiation environment on the surface of the Moon, and the amount of radiation to which astronauts can be exposed.
Another important concept for students to understand is space weather. Space weather refers to the conditions and processes
occurring in space that have the potential to aect spacecraft or people in the space environment. Space weather processes include
changes in the interplanetary magnetic eld, coronal mass ejections, disturbances in the Earth’s magnetic eld, and changes in the
solar wind (energy that ows from the Sun in the form of particles like protons or electromagnetic radiation). Help is needed in
deciding the best time to travel in space, and which materials should be used for the spacesuits, spacecraft, and habitation units
on the Moon. To provide useful planning and launch date recommendations, students will also need to understand how the Sun’s
activity aects the radiation environment in the solar system.
Figure 2: An Apollo astronaut explores the lunar surface.
4 ht tp://quest.nasa.gov/lunar/outpostchallenge/index.html

1
Space Faring: The Radiation Challenge
Radiation
What Is Radiation?
Radiation is a form of energy that is emitted or transmitted in the form of rays, electromagnetic waves, and/or particles. In some
cases, radiation can be seen (visible light) or felt (infrared radiation), while other forms like x-rays and gamma rays are not visible
and can only be observed directly or indirectly with special equipment. Although radiation can have negative eects both on bio-
logical and mechanical systems, it can also be carefully used to learn more about each of those systems.
e motion of electrically charged particles produces electromagnetic waves. ese waves are also called “electromagnetic radia-
tion” because they radiate from the electrically charged particles. ey travel through empty space as well as through air and other
substances. Scientists have observed that electromagnetic radiation has a dual “personality.” Besides acting like waves, it acts like a
stream of particles (called photons) that has no mass. e photons with the highest energy correspond to the shortest wavelengths
and vice versa. e full range of wavelengths (and photon energies) is called the electromagnetic spectrum (shown in gure 3). e
shorter the wavelength, the more energetic the radiation and the greater the potential for biological harm.
1 1 to 10
-3
10
-3
to 10
-6
8 × 10
-7
to 4
× 10
-7
3 × 10
-7
to 10
-8
10
-8
to 10
-12
10
-12
The Electromagnetic Spectrum
Wavelength in Meters
Radio Microwave Infrared Visible Ultraviolet X-ray Gamma Ray
About the size of:
Buildings
Non Ionizing
Radiation
Ionizing
Radiation
Grains
of sugar
Protozoans Bacteria Molecules Atoms Atomic
nuclei
Figure 3: The Electromagnetic Spectrum
On Earth we are protected from much of the electromagnetic radiation that comes from space by Earth’s atmosphere and magnetic
eld. Most radiation is unable to reach the surface of the Earth except at limited wavelengths, such as the visible spectrum, radio
waves, some ultraviolet wavelengths, and some high-energy ionizing radiation. As we rise through the atmosphere, climb a high
mountain, take a plane ight, or go to the ISS or to the Moon, we rapidly lose the protection of the atmosphere.
Where Does Radiation Come From?
In our daily lives we are exposed to electromagnetic radiation through the use of microwaves, cell phones, and diagnostic medical
applications such as x-rays. In addition to human-created technologies that emit electromagnetic radiation such as radio transmit-
ters, light bulbs, heaters, and gamma ray sterilizers (tools that kill microbes in fresh or packaged food), there are many naturally
occurring sources of electromagnetic and ionizing radiation. ese include radioactive elements in the Earth’s crust, radiation
trapped in the Earth’s magnetic eld, stars, and other astrophysical objects like quasars or galactic centers.
Earth’s biggest source of radiation is the Sun. e Sun emits all wavelengths in the electromagnetic spectrum. e majority is in
the form of visible, infrared, and ultraviolet radiation (UV). Occasionally, giant explosions called solar ares and coronal mass ejec-
tions (CME) occur on the surface of the Sun and release massive amounts of energy out into space in the form of x-rays, gamma

2
Space Faring: The Radiation Challenge
rays, and streams of protons and electrons called solar particle events (SPE).
5
A robotic spacecraft called the Solar and Heliospheric
Observatory (SOHO) captured an erupting CME from the surface of the Sun in the image in gure 4
6
. Note the Earth inset at
the approximate scale of the image. ese CME can have serious consequences on astronauts and their equipment, even at loca-
tions that are far from the Sun.
What Are the Different Kinds of Radiation?
Radiation can be either non-ionizing (low energy) or ionizing (high energy). Ionizing radiation consists of particles or photons
that have enough energy to ionize an atom or molecule by completely removing an electron from its orbit, thus creating a more
positively charged atom. Less energetic non-ionizing radiation does not have enough energy to remove electrons from the mate-
rial it traverses. Examples of ionizing radiation include alpha particles (a helium atom nucleus moving at very high speeds), beta
particles (a high-speed electron or positron), gamma rays, x-rays, and galactic cosmic radiation (GCR). Examples of non-ionizing
radiation include radio frequencies, microwaves, infrared, visible light, and ultraviolet light. While many forms of non-ionizing
and ionizing radiation have become essential to our everyday life, each kind of radiation can cause damage to living and non-living
objects, and precautions are required to prevent unnecessary risks.
Figure 4: Erupting CME from the surface of the Sun.
5 ht tp://solarscience.msfc.nasa.gov/CMEs.shtml
6 ht tp://w w w.nasa.gov/vision/universe/solarsystem/perfect_space_storm.html

3
Space Faring: The Radiation Challenge
Why Is Ionizing Radiation More Dangerous Than Non-Ionizing Radiation?
While non-ionizing radiation is damaging, it can easily be shielded out of an environment as is done for UV radiation. Ionizing
radiation, however, is much more dicult to avoid. Ionizing radiation has the ability to move through substances and alter them
as it passes through. When this happens, it ionizes (changes the charge of) the atoms in the surrounding material with which it
interacts. Ionizing radiation is like an atomic-scale cannonball that blasts through material, leaving signicant damage behind.
More damage can also be created by secondary particles that are propelled into motion by the primary radiation particle. e
particles associated with ionizing radiation are categorized into three main groups relating to the source of the radiation: trapped
radiation belt particles (Van Allen Belts), cosmic rays, and solar are particles.
7
What Is Galactic Cosmic Radiation?
Galactic Cosmic Radiation, or GCR, comes from outside the solar system but primarily from within our Milky Way galaxy. In
general, GCR is composed of the nuclei of atoms that have had their surrounding electrons stripped away and are traveling at
nearly the speed of light. Another way to think of GCR would be to imagine the nucleus of any element on the periodic table
from hydrogen to uranium. Now imagine that same nucleus moving at an incredibly high speed. e high-speed nucleus you are
imagining is GCR. ese particles were probably accelerated within the last few million years by magnetic elds of supernova rem-
nants (but not the supernova explosion itself). e giant expanding clouds of gas and magnetic elds that remain after a supernova
can last for thousands of years.
8
During that time, cosmic rays were probably accelerated inside them. e action of the particles
bouncing back and forth in the magnetic eld of the supernova remnant randomly causes some of the particles to gain energy and
become cosmic rays.
9
Eventually they build up enough speed that the remnant can no longer contain them and they escape into
the galaxy. As they travel through the very thin gas of interstellar space, some of the GCR interacts with the gas and emits gamma
rays. Detection of that reaction is how we know that GCR passes through the Milky Way and other galaxies.
e GCR permeates interplanetary space and is comprised of roughly 85% hydrogen (protons), 14% helium, and about 1% high-
energy and highly charged ions called HZE particles. An HZE is a heavy ion having an atomic number greater than that of helium
and having high kinetic energy. Examples of HZE particles include carbon, iron, or nickel nuclei (heavy ions). ough the HZE
particles are less abundant, they possess signicantly higher ionizing power, greater penetration power, and a greater potential for
radiation-induced damage.
10
GCR is extremely damaging to materials and biology. In general, we are largely shielded from GCR
on Earth because of our planet’s atmosphere and magnetic eld, whereas the Moon is not shielded from GCR because it lacks a
global magnetic eld and atmosphere.
In summary, GCR are heavy, high-energy ions of elements that
have had all their electrons stripped away as they journeyed
through the galaxy at nearly the speed of light. ey can cause
the ionization of atoms as they pass through matter and can pass
practically unimpeded through a typical spacecraft or the skin of
an astronaut. e GCR are a dominant source of radiation that
must be dealt with aboard current spacecraft and future space mis-
sions within our solar system. Because these particles are aected
by the Sun’s magnetic eld, their average intensity is highest during
the period of minimum sunspots when the Sun’s magnetic eld is
weakest and less able to deect them. Also, because GCR are dif-
cult to shield against and occur on each space mission, they are
often more hazardous than occasional solar particle events.
11
Figure
5 shows GCR falling onto the surface of Mars. GCR appear as
faint white dots, whereas stars appear as white streaks.
Figure 5: GCR appear as dots in this image. Image credit: NASA.
7 ht tp://see.msfc.nasa.gov/ire/iretech.htm
8 ht tp://helios.gsfc.nasa.gov/gcr.html
9 ht tp://imagine.gsfc.nasa.gov/docs/science/know_l1/cosmic_rays.html
10 ht tp://hrp.jsc.nasa.gov/?viewFile=program/srp
11 w w w.spaceight.nasa.gov/spacenews/factsheets/pdfs/radiation.pdf

4
Space Faring: The Radiation Challenge
Are We Protected from Space Radiation on Earth?
Yes, but not entirely. Life on Earth is protected from the full impact of solar and cosmic radiation by the magnetic elds that sur-
round the Earth and by the Earth’s atmosphere. e Earth also has radiation belts caused by its magnetic eld. e inner radiation
belt or Van Allen Belt consists of ionizing radiation in the form of very energetic protons—by-products of collisions between GCR
and atoms of Earth’s atmosphere. e outer radiation belts contain ions and electrons of much lower energy. As we travel farther
from Earth’s protective shields we are exposed to the full radiation spectrum and its damaging eects.
12
In addition to a protective atmosphere, we are also lucky that Earth has a magnetic eld. It shields us from the full eects of the
solar wind and GCR. Without this protection, Earth’s biosphere might not exist as it does today, or would be at least limited to
the subsurface. e small blue torus near the Earth in gure 6
13
is the approximate location of the Van Allen Belts, where high-
energy radiation is trapped.
Figure 6: Van Allen Belts.
Image Credit: NASA.
12 ht tp://w w w-istp.gsfc.nasa.gov/Education/Iradbelt.html
13 ht tp://science.msfc.nasa.gov/ssl/pad/solar/images/sunearth_lg.gif

5
Space Faring: The Radiation Challenge
What Factors Determine the Amount of Radiation Astronauts Receive?
ere are three main factors that determine the amount of radiation that astronauts receive. ey include:
14
• Altitude above the Earth – at higher altitudes the Earth’s magnetic eld is weaker, so there is less protection against ionizing
particles, and spacecraft pass through the trapped radiation belts more often.
• Solar cycle – the Sun has an 11-year cycle, which culminates in a dramatic increase in the number and intensity of solar ares,
especially during periods when there are numerous sunspots.
• Individual’s susceptibility – researchers are still working to determine what makes one person more susceptible to the eects
of space radiation than another person. is is an area of active investigation.
Does Space Weather Affect Astronauts?
Absolutely. Space weather is closely related to solar activity and this is important for astronauts traveling through space. Scientists have
discovered that over an 11-year cycle the number of sunspots increase and decrease as shown in gure 7.
15
Interestingly, the Sun is
slightly brighter when there are many sunspots. During one of these periods, the Sun is more actively producing SPE and CME so the
amount of radiation in the solar system is slightly increased. e number of CMEs varies with the solar cycle, going from about one
per day at solar minimum, up to two or three per day at solar maximum. Although scientists can predict that the Sun can produce
more SPE and CME during this period, they are unable to determine specically when SPE and CME will occur.
14 w w w.spaceight.nasa.gov/spacenews/factsheets/pdfs/radiation.pdf
15 ht tp://solarscience.msfc.nasa.gov/images/zurich.gif
Figure 7: The sunspot cycle of the Sun.
Image credit: NASA.
Monthly Average Sunspot Number
300
200
100
0
300
200
100
0
300
200
100
0
1750 1760 1770 1780 1790 1800
Date
1810 1820 1830 1840 1850
1850 1860 1870 1880 1890 1900
Date
1910 1920 1930 1940 1950
1950 1960 1970 1980 1990 2000
Date
2010 2020 2030 2040 2050

6
Space Faring: The Radiation Challenge
Because the levels of protection vary, the radiation environments vary between planets and moons, even at dierent places on the sur-
face of individual planets. e ISS has well-shielded areas. In addition, astronauts and the ISS itself are largely protected by the Earth’s
magnetic eld because it is in low Earth orbit. In contrast, during a deep space journey to the Moon (240,000 miles or 385,000
kilometers away) or Mars (35,000,000 miles or 56,300,000 kilometers away at closest approach), astronauts and their vehicles will
venture far outside of the 30,000-mile radius of the Earth’s protective magnetic shield. For any future long-duration deep-space explo-
ration, radiation levels will be so high that specially designed storm shelters will be needed to protect astronauts from receiving deadly
doses of radiation during high SPE/CME periods. For safe operations on the Moon or when traveling to Mars, a coordinated system
of satellites will be needed to monitor space weather to help warn astronauts when it is necessary to go into their shelters.
16
is is
because, although increases and decreases in overall solar activity can be fairly well predicted over an 11-year cycle, there are unex-
pected short-term events like solar ares, SPE, and CME that cannot be predicted, which would put a crew in great danger.
How Is Radiation Measured?
ere are several properties of radiation that must be considered when measuring or quantifying radiation. ese include the
magnitude of radioactivity of the source, the energy of the radiation itself, the amount of radiation in the environment, and the
amount of radiation energy that is absorbed. Collectively, these properties determine the nature of the radiation itself. It is very
important to understand that equal doses of dierent kinds of radiation are not equally damaging. To account for the dierence,
radiation dose is expressed as “dose equivalent.” Table 1 summarizes each parameter:
Table 1: Dose equivalent chart.
Parameter
Radioactivity Absorbed Dose Dose Equivalent*
Exposure (for x-rays
and gamma rays only)
Energy
Denition
Rate of radiation emis-
sion (transformation or
disintegration) from a
radioactive substance
Energy imparted
by radiation per
unit mass onto an
absorbing material
Expression of dose
in terms of its
biological effect
Quantity that expresses
the ability of radiation
to ionize air and thereby
create electric charges
that can be collected
and measured
The capacity
to do work
Common Units
Measurement
Label
curie (Ci)
1 Ci = 37 GigaBq (this
is a large amount)
rad
1 rad = 100 ergs/g
rem roentgen (R) joule (J)
International
System of Units
(SI) Measure-
ment Label
becquerel (Bq)
1 Bq = 1 event of
radiation emission per
second
(this is a very small
amount)
Gray (Gy)
1 Gy = 100 rad
sievert (Sv)
1 Sv = 100 rem
(this is a large dose)
1 Gy air dose
equivalent = 0.7 Sv
1 R ≈ 10 mSv of tissue
dose
coulomb/kilogram
(C/kg)
1 R = 2.58 × 10
-4
C/kg air
electronvolts (eV)
*DE = Absorbed Dose × Quality Factor (Q), where Q depends on the type of radiation
Q = 1 for gamma, x-ray, or beta radiation; Q = 20 for alpha radiation
When measuring radiation energy another consideration is that equal doses of all types of ionizing radiation do not produce the same
harmful biological eects. In particular, alpha particles (the nuclei of the helium atom) exert more damage than do beta particles,
gamma rays, and x-rays for a given absorbed dose depositing their energy thousands of times more eectively. While lower energy
electrons can pass through the spacing between DNA strands without interacting, some high-energy heavy ions produce an ionization
trail so intense that it can kill nearly every cell it traverses (see the radiation damage in the living organisms section for more detail).
16 ht tp://marsprogram.jpl.nasa.gov/spotlight/odyssey-mission-success.html

7
Space Faring: The Radiation Challenge
To account for the dierence in harmful eects produced by dierent types of ionizing radiation, radiation dose is expressed as
dose equivalent. e unit of dose equivalent is the sievert (Sv). e dose in Sv is equal to “absorbed dose” multiplied by a “radia-
tion weighting factor” that was previously known as the Quality Factor (Q). Historically, x-rays have been used as the standard ref-
erence radiation against which all other types of radiation have been compared so the weighting factor for x-rays and gamma rays
is 1. Since alpha particles cause 20 times the damage of a similar dose of x-rays or gamma rays, they have a Q of 20.
Some books use the rem to measure dose equivalent. One Sv, or 100 rem of radiation, is presumed, for the purpose of radiation
protection, to have the same biological consequences as 1 Gray (Gy) of x-rays. Although there are exceptions, in general when
radiation energy is transferred, the deposited energy (absorbed dose) is closely related to the energy lost by the incident particles.
17
e energy imparted is expressed in the unit Gy, which is equivalent to one joule of radiation energy absorbed per kilogram of
organ or tissue weight. However, it should be noted that an older unit — the rad — is still frequently used to express absorbed dose;
one Gy is equal to 100 rad.
Are There Radiation Exposure Limits?
Yes. e specic organ and career exposure limits are determined by one’s age and gender. e typical average dose for a person
is about 360 mrems per year, or 3.6 mSv, which is a small dose. However, International Standards allow exposure to as much as
5,000 mrems (50 mSv) a year for those who work with and around radioactive material. For spaceight, the limit is higher. e
NASA limit for radiation exposure in low-Earth orbit is 50 mSv/year, or 50 rem/year. Note that the values are lower for younger
astronauts as seen in table 2. Since it is presumed that, although they may live longer than older astronauts, exposure to larger
amounts of radiation early in their careers could present greater health risks during old age.
Table 2: Exposure limits for NASA astronauts.
Career Exposure Limits for NASA Astronauts by Age and Gender*
Age (years) 25 35 45 55
Male 1,500 mSv 2,500 mSv 3,250 mSv 4,000 mSv
Female 1,000 mSv 1,750 mSv 2,500 mSv 3,000 mSv
* Please visit the website for more information on radiation exposure limits.
18
e career depth equivalent dose limit is based upon a maximum 3% lifetime excess risk of cancer mortality. e total equivalent
dose yielding this risk depends on gender and age at the start of radiation exposure. Assume that a younger person can be exposed
to less radiation because they have more life to live, and therefore a longer chance to develop subsequent health problems. Table 3
compares the specic exposure limits between the general public and astronauts. Astronauts who spend three months in the ISS
will be subjected to over three times the maximum recommended dosage of radiation for one year.
17 For example, high-energy electrons produced by charged particles traversing a cell may escape, to deposit their energy in other locations, outside the cell. At
low dose rates, only one or a few particles are likely to traverse a cell. e energy deposited in the cell is less than the energy lost by the particles. However,
when a large number of particles are present, then electrons generated outside the cell may compensate for those that are lost. us, the concept of absorbed
dose incorporates many assumptions and approximations.
18 ht tp://srag.jsc.nasa.gov/Publications/TM104782/techmemo.htm

8
Space Faring: The Radiation Challenge
Table 3: Radiation penetration and exposure limits.
Depth of Radiation Penetration and Exposure Limits
for Astronauts and the General Public (in mSv)
Exposure
Interval
Blood Forming Organs
(5 cm depth)
Eyes
(0.3 cm depth)
Skin
(0.01 cm depth)
Astronauts
30 Days 250 1,000 1,500
Annual 500 2,000 3,000
Career 1,000-4,000 4,000 6,000
General Public Annual 1 1,500 50
Table 4 compares and contrasts various missions and their durations with the observed radiation dose:
Table 4: Missions and radiation dose.
Mission Type Radiation Dose
Space Shuttle Mission 41-C
(8-day mission orbiting the Earth at 460 km)
5.59 mSv
Apollo 14
(9-day mission to the Moon)
11.4 mSv
Skylab 4
(87-day mission orbiting the Earth at 473 km)
178 mSv
ISS Mission
(up to 6 months orbiting Earth at 353 km)
160 mSv
Estimated Mars mission (3 years) 1,200 mSv
Crews aboard the Space Station receive an average of 80 mSv for a six-month stay at solar maximum (the time period with the
maximum number of sunspots and a maximum solar magnetic eld to deect the particles) and an average of 160 mSv for a six-
month stay at solar minimum (the period with the minimum number of sunspots and a minimum solar magnetic eld). Although
the type of radiation is dierent, 1 mSv of space radiation is approximately equivalent to receiving three chest x-rays. On Earth, we
receive an average of 2 mSv every year from background radiation alone.
19
19 w w w.spaceight.nasa.gov/spacenews/factsheets/pdfs/radiation.pdf

9
Space Faring: The Radiation Challenge
How Does the Radiation Environment on Earth Compare
to the Radiation Environment on the Moon and Mars?
NASA has collected a variety of radiation and environmental
data from the Moon and Mars. During the Lunar Prospector
mission, NASA scientists discovered that there are some areas
of the Moon that have a weak magnetic eld. Magnetic elds
have the ability to deect small amounts of radiation. Locations
with these elds are slightly more protected and might be can-
didate sites for bases on the Moon. Mars also has similar mag-
netic elds, though greater than those of the Moon. As shown in
gure 8, the strongest magnetic elds on the Moon are located
at ≈20˚S, 170˚E and ≈43˚S, 170˚E. e Lunar Reconnaissance
Orbiter will continue to measure magnetic elds on the Moon
beginning in 2008.
e Moon and Mars are still extremely vulnerable to the eects
of space radiation in spite of localized magnetic elds. ey do
not have global magnetic elds like those of Earth. As a result,
their surfaces are not shielded from SPE that erupt from the sur-
face of the Sun. In addition, the GCR that permeates interstellar
space can freely bombard the surface of the Moon and Mars.
Finally, the Moon and Mars do not have dense atmospheres.
Although Mars has an extremely thin atmosphere composed pri-
marily of carbon dioxide, it is not thick enough to shield it from
most cosmic radiation. e Moon essentially lacks an atmosphere
altogether.
In order to minimize radiation exposure, people living on the
Moon or Mars will need to limit the time they spend outside in their spacesuits and the distance they travel from their protective
habitats. e total amount of radiation that astronauts receive will greatly depend upon solar activity, their location with respect
to planetary magnetic elds, and the amount and type of radiation shielding used in habitats and spacecraft. Radiation exposure
for astronauts aboard the ISS in Earth orbit is typically equivalent to an annualized rate of 20 to 40 rems (200 – 400 mSv).
20
e
average dose-equivalent rate observed on a previous Space Shuttle mission was 3.9 µSv/hour, with the highest rate at 96 µSv/hour,
which appeared to have occurred while the Shuttle was in the South Atlantic Anomaly region of Earth’s magnetic eld (1 Sv =
1,000 mSv = 1,000,000 µSv).
21
For a six-month journey to Mars an astronaut would be exposed to roughly 300 mSv, or a total of 600 mSv for the round-trip.
If we assume that the crew would spend 18 months on the surface while they wait for the planets to realign to make the journey
back to Earth possible, they will be exposed to an additional 400 mSv, for a grand total exposure of about 1,000 mSv. Note that
an astronaut repeating the same journey on multiple occasions could receive less or more radiation each time, if they are in the line
of a CME or SPE.
-20
Latitude (deg)
Reflection coefficient
East Longitude (deg)
-40
-60
-80
0.78
0.60
0.42
0.25
0.07
170 180 190 200 210
Figure 8: Magnetic elds on the moon.
Image credit: NASA.
20 ht tp://hrp.jsc.nasa.gov/?viewFile=program/srp
21 ht tp://w w w.nasa.gov/mission_pages/station/science/experiments/BBND.html

10
Space Faring: The Radiation Challenge
Name: Date:
Pretest Activity: Ionizing, Non-Ionizing, or Both?
e following objects and medical procedures produce or use radiation. Your task is to classify items 1-16 as using or producing
ionizing radiation, non-ionizing radiation, or both. Place an “✗” in the column that correctly identies the type of radiation
produced or used for each. Finally, circle the picture of those that emit particle radiation.
1. 2. 3. 4.
5. 6. 7. 8.
9. 10. 11. 12.
13. 14. 15. 16.
Object or Medical Procedure
Type of Radiation Produced or Used
Ionizing Non-Ionizing Both
1. Cell phone
2. Laptop computer
3. Chest x-ray
4. Abdomen CT scan*
5. Remote Control
6. Tanning Bed
7. Skull MRI*
8. Flat Panel Screen
9. Television (tube type)
10. Sun
11. Microwave
12. Supernova
13. Dental x-ray machine
14. Earth
15. Ultrasound of a baby
16. Atomic bomb
*CT = Computed Tomography
*MRI = Magnetic Resonance Image

11
Space Faring: The Radiation Challenge
Name: Date:
Pretest Activity: Ionizing, Non-Ionizing, or Both? Answers
e following objects and medical procedures produce or use radiation. Your task is to classify items 1-16 as using or producing
ionizing radiation, non-ionizing radiation, or both. Place an “✗” in the column that correctly identifies the type of radiation
produced or used for each. Finally, circle the picture of those that emit particle radiation.
1. 2. 3. 4.
5. 6. 7. 8.
9. 10. 11. 12.
13. 14. 15. 16.
Object or Medical Procedure
Type of Radiation Produced or Used
Ionizing Non-Ionizing Both
1. Cell phone
✗
2. Laptop computer
✗
3. Chest x-ray
✗
4. Abdomen CT scan*
✗
5. Remote Control
✗
6. Tanning Bed
✗
7. Skull MRI*
✗
8. Flat Panel Screen
✗
9. Television (tube type)
✗
10. Sun
✗
11. Microwave
✗
12. Supernova
✗
13. Dental x-ray machine
✗
14. Earth
✗
15. Ultrasound of a baby
✗
16. Atomic bomb
✗
*CT = Computed Tomography
*MRI = Magnetic Resonance Image

12
Space Faring: The Radiation Challenge
Name: Date:
Pretest Activity: Matching Radiation Doses – Directions: e bars in the graph below compare nine
dierent radiation doses received during events A through I. Your task is to write the correct letter of the event in the line below
the bar that represents the radiation dose for that event. e letter choices of the events are:
(A) Nine days on the Moon
(B) One single CAT scan of body
(C) One single chest x-ray
(D) Eight days on the Space Shuttle
(E) A single dental x-ray exposure to your arm, hand, foot or leg
(F) A single upper GI x-ray
(G) A single skull/neck x-ray
(H) A single pelvis/hip x-ray
(I) One year of normal radiation on Earth
0
2
4
6
8
10
12
1 2 3 4 5 6 7 8 9
Radiation Dose Per Event
Answers:
Event
Dose (in mSv)

13
Space Faring: The Radiation Challenge
Name: Date:
Pretest Activity: Matching Radiation Doses – Answers: e bars in the graph below compare nine
dierent radiation doses received during events A through I. Your task is to write the correct letter of the event in the line below
the bar that represents the radiation dose for that event. e letter choices of the events are:
(A) Nine days on the Moon
(B) One single CAT scan of body
(C) One single chest x-ray
(D) Eight days on the Space Shuttle
(E) A single dental x-ray exposure to your arm, hand, foot or leg
(F) A single upper GI x-ray
(G) A single skull/neck x-ray
(H) A single pelvis/hip x-ray
(I) One year of normal radiation on Earth
0
2
4
6
8
10
12
1 2 3 4 5 6 7 8 9
Radiation Dose Per Event
Answers:
Event
Dose (in mSv)
E C G H B F I D A

14
Space Faring: The Radiation Challenge
Activity I: Radiation Exposure on Earth
In Activity I, students will use worksheets to determine their average annual radiation dose here on Earth.
Background
Radiation is a form of energy that is emitted or transmitted in the form of rays, electromagnetic waves, and/or particles. In some cases,
radiation can be seen (visible light) or felt (infrared radiation), while other forms like x-rays and gamma rays are not visible and can
only be observed directly or indirectly with special equipment. Although radiation can have negative eects both on biological and
mechanical systems, it can also be carefully used to learn more about each of those systems.
On Earth we are protected from much of the electromagnetic radiation that comes from space by Earth’s atmosphere and magnetic
eld. Most radiation is unable to reach the surface of the Earth except at limited wavelengths, such as the visible spectrum, radio
waves, some ultraviolet wavelengths, and some high-energy ionizing radiation. As we rise through the atmosphere, climb a high
mountain, take a plane ight, or go to the International Space Station (ISS) or to the Moon, we rapidly lose the protection of the
atmosphere and magnetic eld.
Please see the introduction for more background about radiation.
Objectives:
By the end of this lesson, the students will be able to:
• Explain that radiation exposure on Earth is determined mainly by where people live, how people live (lifestyle), and by the
medical procedures people have experienced.
• Determine their average annual radiation dose here on Earth.
• Describe some medical procedures that increase their radiation exposure.
• Explain the dierence between acute and chronic radiation exposure.
• Compare their radiation exposure to an astronaut’s radiation exposure.
Research Question:
How does your radiation exposure compare to an astronaut’s radiation exposure, and why are they dierent?
Discussion Questions:
Regarding a human-tended lunar outpost, have students discuss in detail how and why radiation might aect the total duration
astronauts can stay on the Moon. Other possible topics for discussion include:
• What are the dierent kinds of radiation?
• What units are used to describe radiation exposure?
• What is your annual radiation exposure?
• How does your radiation exposure compare to an Apollo 14 astronaut (use chart)?
• Are you exposed to radiation when watching TV?
• How does your altitude (height above sea level) aect your radiation exposure?
• What are some examples of medical procedures that are high in radiation?
• Does where you live on the Earth aect your radiation exposure?
• Does the Earth give o radiation?
• How can you reduce the amount of radiation you are exposed to?
• Why is radiation exposure more for ISS astronauts than for Space Shuttle astronauts?
• What kind of health eects due to radiation might Moon and Mars explorers experience?

15
Space Faring: The Radiation Challenge
National Education Standards
22
:
Unifying Concepts and Processes
Systems, order, and organization
Evidence, models, and explanation
Science in Personal and Social Perspectives
Natural hazards
Personal health
Science and technology in society
Physical Science
Transfer of energy
Earth and Space Science
Structure of the Earth system
Materials:
Provide to the students the spaceight radiation examples chart (Chart I), the acute radiation exposure chart that gives examples of
health eects (Chart II), a short glossary of terms, and the Radiation Exposure on Earth worksheet. Show the comparison of radia-
tion examples (Chart III and graphs) to students so they can visualize the dierences between them.
Note: 1 Sv = 1,000 mSv.
Time allotment: 90 – 120 minutes
References:
1. e chart for calculating a personal radiation dose was derived in part from the American Nuclear Society’s brochure titled
Personal Radiation Dose.
e primary sources for this information are National Council on Radiation Protection and Measurements Reports: #92
Public Radiation Exposure from Nuclear Power Generation in the United States (1987); #93 Ionizing Radiation Exposure of
the Population of the United States (1987); #94 Exposure of the Population in the United States and Canada from Natural
Background Radiation (1987); #95 Radiation Exposure of the U.S. Population from Consumer Products and Miscellaneous
Sources, (1987); and #100 Exposure of the U.S. Population from Diagnostic Medical Radiation (1989).
2. e Environmental Protection Agency has established Radiation Protection Programs that are responsible for preparing regula-
tions and guidance on protective limits. Health eects are the central focus in establishing the limits. is site explains the top-
ics that the EPA considers.
ht tp://w w w.epa.gov/radiation/understand/health_eects.htm
3. For more information about radiation health aects, also see:
ht tp://srag.jsc.nasa.gov/SpaceRadiation/FAQ/FAQ.cfm
Going Further:
For additional research opportunities, have students investigate:
• Case studies of radiation exposure in people from the workplace, cell phones, nuclear explosions, radon, or nuclear power
plant meltdowns.
• e concept of “half-life.”
• NASA’s use of radiation facilities at Brookhaven National Lab and Loma Linda University.
• e history of the discovery of radiation, and the scientists Marie Curie and Pierre Curie.
22 National Science Education Standards, Center for Science, Mathematics, and Engineering Education (CSMEE), National Academy of Sciences, National
Academy Press, Washington, DC., 1996, ISBN 0-309-05326-9.

16
Space Faring: The Radiation Challenge
Chart I. Spaceight Radiation Examples
Human Spaceight Mission Type Radiation Dose
Space Shuttle Mission 41-C
(8-day mission orbiting the Earth at 460 km)
5.59 mSv
Apollo 14
(9-day mission to the Moon)
11.4 mSv
Skylab 4
(87-day mission orbiting the Earth at 473 km)
178 mSv
International Space Station (ISS) Mission
(up to 6 months orbiting Earth at 353 km)
160 mSv
Estimated Mars mission (3 years) 1200 mSv
Note: units of exposure on this chart are in milliSieverts (mSv). 1 Sv = 1000 mSv.
Chart II. Examples of Health Effects from
Acute Radiation Exposure
Exposure (mSv) Acute Health Effects
*
Time to Onset (without
treatment)
Less than 100 No detectable health effects
Above 100 Cell and chromosomal (DNA) damage hours
Above 1,000 Nausea, vomiting, diarrhea: prodromic syndrome
1 to 2 days
Above 1,500
Damage to blood-forming organs: hematopoietic
syndrome; possible death
≈1 month
3,000 50% death from hematopoietic syndrome in 30 to 60 days
10,000
Destruction of intestinal lining
Internal bleeding
Death 1-2 weeks
20,000
Damage to central nervous system
Loss of consciousness minutes
Death hours to days
Note: units of exposure on this chart are in Sieverts (Sv). 1 Sv = 1,000 mSv.
* e acute eects in this table are cumulative. For example, a dose that causes damage to bone marrow will produce changes
in blood chemistry and be accompanied by nausea. At a certain threshold every individual will experience these kinds of eects,
which include nausea, skin reddening, sterility, and cataract formation.

17
Space Faring: The Radiation Challenge
Chart III. Comparison of Radiation Doses
Description Exposure (mSv)
A single dental, arm, hand, foot, or leg x-ray 0.01
A single chest x-ray 0.06
A single skull/neck x-ray 0.2
A single pelvis/hip x-ray 0.65
A single CAT scan of body 1.1
A single upper GI x-ray 2.45
One year of normal radiation on Earth (approximate) 3.0
8 days on the Space Shuttle 5.59
9 days on the Moon 11.4
6 months on the International Space Station 160
Lowest dose received during 1945 Hiroshima bomb
Estimated dose for a 3-y
ear round trip for a Mars Mission
200
1,200
Note: e items in Chart III are plotted in Graph 1 (see next page).

18
Space Faring: The Radiation Challenge
Comparison of Radiation Doses
0
200
400
600
800
1000
1200
one single dental, arm, hand, foot, or leg x-ray
one single chest x-ray
One single skull/neck x-ray
one single pelvis/hip x-ray
one single CAT Scan of body
one single upper GI x-ray
one year of normal radiation on Earth
8 days on the Space Shuttle
9 days on the Moon
6 months on the International Space Station
Lowest dose received during 1945 Hiroshima bomb
Estimated dose for a 3-year Mars mission
Radiation Dose (mSv)
Type of Radiation Exposure or Event
Graph 1: A comparison of radiation doses.

19
Space Faring: The Radiation Challenge
Radiation Exposure on Earth
Name: Date:
Directions:
Estimate your annual radiation dose by adding together the amount of radiation you are exposed to from
common sources of radiation. Place the value from the “Common Sources of Radiation” column (middle column) that corre-
sponds to your situation in the “Annual Dose” column (right column). All values are in milliSieverts (mSv). Add all of the num-
bers in the right column to determine your total estimated annual radiation dose. Answer the discussion questions.
Factors Common Sources of Radiation Annual Dose
Where You Live
Cosmic Radiation (from outer space)
Exposure depends on your elevation (how much atmosphere is above you to block radiation). _________mSv
Elevation
(average cities’ data from the United States Geological Survey web- Value (mSv)
site: ht tp://w w w.usgs.gov)
Sea level (New York, Philadelphia, Houston, Baltimore, Boston, New Orleans, 0.26
Jacksonville, Seattle)
1-1,000 feet (Chicago, Detroit, San Diego, Dallas, Minneapolis, St. Louis, 0.28
Indianapolis, San Francisco, Memphis, Washington, DC, Milwaukee, Cleveland,
Columbus, Atlanta)
1,001-2,000 feet (Phoenix, Pittsburgh, San Jose, Oklahoma City) 0.31
2,001-3,000 feet
(Las Vegas, Los Angeles, Honolulu, Tucson) 0.35
3,001-4,000 feet
(El Paso) 0.41
4,001-5,000 feet
(Salt Lake City) 0.47
5,001-6,000 feet
(Denver, Albuquerque) 0.52
6,001-7,000 feet 0.66
7,001-8,000 feet 0.79
8,001-9,000 feet 0.96
Terrestrial Radiation (from the ground)
• If you live in a state that borders the Gulf of Mexico or Atlantic Ocean, add 0.16 mSv.
• If you live in the Colorado Plateau area (around Denver), add 0.63 mSv. _________mSv
• If you live anywhere else in the continental U.S., add 0.30 mSv.
House Construction
• If you live in a stone, adobe, brick, or concrete building, add 0.07 mSv. _________mSv
Power Plants
• If you live within 50 miles of a nuclear power plant, add 0.0001 mSv. (For locations of nuclear
power plants, visit the United States Nuclear Regulatory Commision website: ht tp://w w w.nrc.
gov/info-ner/reactor) _________mSv
• If you live within 50 miles of a coal-red power plant, add 0.0003 mSv.
Food
Internal Radiation (average values) ______
0.40
⁄
mSv
Water
• From food (most food has naturally occurring radioactive Carbon-14 and Potassium-40) and
Air
from water (radon dissolved in water).
• From air (radon emanating from the ground).
______
2.00
⁄
mSv
Total
Add all the values for your annual radiation dose in the third column. _________mSv

20
Space Faring: The Radiation Challenge
Factors Common Sources of Radiation Annual Dose
Total (page 1)
Transfer the total from the previous page onto this line.
_________mSv
How You Live
Add the following values if they apply to you:
Live near a weapons test fallout site 0.01 mSv _________mSv
Jet plane travel 0.005 mSv per hour
in the air (total for all
ights in one y
ear)
_________mSv
If you have porcelain crowns or false teeth 0.0007 mSv per tooth/
cro
wn (2 crowns =
0.0014 mSv)
_________mSv
If you wear a luminous wrist-watch 0.0006 mSv _________mSv
If you watch TV 0.01 mSv _________mSv
If you use a computer screen 0.01 mSv _________mSv
If you have a smoke detector 0.00008 mSv _________mSv
If you use a gas camping lantern 0.002 mSv _________mSv
If you smoke 160.0 mSv _________mSv
Medical Tests
Medical diagnostic tests performed on you this year (per procedure)
Extremity x-ray (arm, hand, foot, or leg) 0.01 mSv (if you had
tw
o x-rays, then =
0.02 mSv)
_________mSv
Dental x-ray 0.01 mSv _________mSv
Chest x-ray 0.06 mSv _________mSv
Pelvis/hip x-ray 0.65 mSv _________mSv
Skull/neck x-ray 0.20 mSv _________mSv
Upper gastro-intestinal x-ray 2.45 mSv _________mSv
CAT scan (head and body) 1.1 mSv _________mSv
Nuclear medicine (e.g. thyroid scan) 0.14 mSv _________mSv
Total
Annual Dose
Add up all of the numbers in the third column of this page.
This is your annual radiation dose on Earth. _________mSv

21
Space Faring: The Radiation Challenge
Name: Date:
Measuring Your Radiation Discussion Questions:
(1a) How do you think your annual radiation dose will compare to your classmates and teacher?
What leads you to that conclusion?
(1b) Why should humans be concerned about radiation on Earth?
(1c) Identify groups of people who may be more concerned about radiation than others.
(1d) What is your annual radiation exposure in mSv?
(2) How does your radiation exposure compare to an Apollo 14 astronaut? How does it compare to an International
Space Station astronaut? Why are the radiation dose values for each mission dierent (use Chart I)?
(3) Are you exposed to radiation when watching TV? Explain.
(4) Why does your altitude aect your radiation exposure? How?
(5) What are some examples of medical procedures that are high in radiation?
(6) Does where you live on the Earth aect your radiation exposure? Why?
(7) What is the dierence between acute and chronic radiation exposure?
(8) How could you reduce the amount of radiation you are exposed to?
(9) Why is radiation exposure more for ISS astronauts than Space Shuttle astronauts?
(10) If astronauts were exposed to an acute radiation dose of 1,010 mSv from a CME while exploring on the Moon, what kinds
of health eects might they experience? (use Chart II)
(11) How does your radiation exposure compare to an astronaut’s radiation exposure, and why are they dierent?
Give three reasons.
(12) Describe three things that aect the magnitude of a radiation dose.

22
Space Faring: The Radiation Challenge
Answer Key Measuring Your Radiation Discussion Questions:
(1a) How do you think your annual radiation dose will compare to your classmates and teacher?
What leads you to that conclusion?
is will vary from student to student and area to area.
(1b) Why should humans be concerned about radiation on Earth?
Radiation causes damage to biological systems and can be potentially harmful (if exposed to large enough doses).
(1c) Identify groups of people who may be more concerned about radiation than others.
People that smoke, live at higher altitudes, are exposed to more medical procedures that use radiation.
(1d) What is your annual radiation exposure in mSv?
is will vary from student to student and area to area.
(2) How does your radiation exposure compare to an Apollo 14 astronaut? How does it compare to an International
Space Station astronaut? Why are the radiation dose values for each mission dierent (use Chart I)?
Student exposure to radiation will be less than Apollo 14 and ISS astronauts. e values for each mission in Chart I are higher
because astronauts are exposed to more radiation than we are on Earth. e altitude of the mission, the mission duration, and the
time frame relative to the sun spot cycle also aect how much radiation astronauts receive. Notice that the longest missions
(in places outside of Earth’s protective atmosphere and magnetic eld) have the highest radiation doses.
(3) Are you exposed to radiation when watching TV?
Yes.
(4) Why does your altitude aect your radiation exposure? How?
Yes — as altitude increases, the amount of radiation you will be exposed to also increases.
(5) What are some examples of medical procedures that are high in radiation?
Diagnostic procedures: upper gastrointestinal X-ray, mid-gastro-intestinal x-ray (esophagus, stomach, and small intestine, usually
done following a barium milkshake), CAT scan; therapeutic procedures: external exposure, where a beam of x-rays, gamma rays,
or electrons are directed at a tumor, or internal exposure, where sealed radioactive sources are inserted into a tumor to produce
a highly focused dose designed to destroy the tumor.
(6) Does where you live on the Earth aect your radiation exposure? Why?
Yes. If your altitude increases, so does your radiation exposure; dierent areas of the Earth also have more naturally occurring
radiation.
(7) What is the dierence between acute and chronic radiation exposure?
Acute exposure is short-term, high-level exposure to radiation. e eects of acute radiation exposure become more severe as the
exposure increases. Health eects from acute exposure to radiation usually appear quickly. e physical response is called radiation
sickness, or radiation poisoning. Chronic exposure is long-term, low-level exposure to radiation. Higher levels of radiation exposure
make these health eects more likely to occur, but do not inuence the type or severity of the eect. Examples of health eects
from chronic radiation damage include cancer, leukemia, and genetic changes.
(8) How could you reduce the amount of radiation you are exposed to?
You can reduce your exposure by, for example, living at low altitudes, and away from other radiation sources, limit the number
of medical procedures that use radiation, and don’t smoke.
(9) Why is radiation exposure more for ISS astronauts than Space Shuttle astronauts?
e duration of spaceight missions for ISS astronauts is longer than Space Shuttle astronauts, therefore, they are exposed to much
more radiation.

23
Space Faring: The Radiation Challenge
(10) If astronauts were exposed to an acute radiation dose of 1,010 mSv from a CME while exploring on the Moon, what kinds
of health eects might they experience?
Radiation sickness and prodromic syndrome (nausea, vomiting, diarrhea).
(11) How does your radiation exposure compare to an astronaut’s radiation exposure, and why are they dierent?
Give three reasons.
Answers will vary, but student exposure values will be less than that of an astronaut. Astronauts have higher radiation exposure
values because they are outside of earth’s protective atmosphere, outside of the majority of Earth’s protective magnetic eld (when
exploring the Moon or Mars), and they are also exposed to more galactic cosmic radiation. Overall, astronauts are exposed to
more of the electromagnetic radiation and particle radiation from both the sun and extrasolar sources.
(12) Describe three things that aect the magnitude of a radiation dose.
ere are many things that aect the magnitude of a radiation dose. For example, proximity to the source of radiation (how
close or far from the source), duration you are exposed to the radiation (chronic or acute exposure), type of radiation (whether
it is particle or electromagnetic radiation), and whether or not you are shielded from the radiation all aect the magnitude
of a radiation dose.

24
Space Faring: The Radiation Challenge
Radiation Damage in Living Organisms
As we have discussed, space radiation can penetrate habitats, spacecraft, equipment, spacesuits, and even astronauts themselves.
e interaction of ionizing radiation with living organisms can lead to harmful health consequences such as tissue damage, cancer,
and cataracts in space and on Earth. e underlying cause of many of these eects is damage to deoxyribonucleic acid (DNA). e
degree of biological damage caused by ionizing radiation depends on many factors such as radiation dose, dose rate, type of radia-
tion, the part of the body exposed, age, and health. In this section, we will discuss the risks and symptoms of space radiation expo-
sure including how and why this radiation causes damage, and how the body works to repair the damage. We will also discuss how
scientists study the eects of radiation on living organisms, and why this research is important to NASA.
Why Is NASA Studying the Biological Effects of Radiation?
NASA wants to keep astronauts safe and healthy during long-duration space missions. To accomplish this challenging task, NASA
has identied four signicant health risks due to radiation that must be well understood to enable the development of eective
countermeasures. e risks are described in the NASA Bioastronautics Critical Path Roadmap, and include carcinogenesis, acute
and late central nervous system risks, chronic and degenerative tissue risks, and acute radiation risks.
23
NASA scientists are working
to understand the molecular, cellular and tissue mechanisms of damage, which include DNA damage processing, oxidative dam-
age, cell loss through apoptosis or necrosis, changes in the extra-cellular matrix, cytokine activation, inammation, changes in plas-
ticity, and micro-lesions (clusters of damaged cells along heavy ion tracks). Knowing this information will help researchers develop
the appropriate countermeasures.
How Do Scientists Study Biological Change During Spaceight?
Because the radiation environment in space is dier-
ent than that on Earth, the biological responses are
dierent. As a result, NASA scientists must develop
space biology experiments that are designed to care-
fully study model organisms in space. In this sce-
nario, the organism is sent into space and allowed
to grow and develop. is part of the experiment is
called the ight experiment. e same experiment is
also repeated on the Earth, and this is called a ground
control, an example of which is shown in gure 1.
Careful analysis of both the ight experiment and
ground controls are critical to understanding the bio-
logical changes that result from spaceight.
Many studies are also carried out in ground-based
research. Opportunities to y experiments can be rare,
and experiments must be well planned. Ground-based
research allows a variety of parameters to be tested so that the investigator can decide which will be the best to focus on in a space-
ight experiment. For radiation studies, ground-based research can also help in identifying the specic biological responses for a par-
ticular radiation source. is is because on Earth, biological experiments can be carried out using a source that simulates just one kind
of radiation, rather than the complex mix of radiation types that make up the space radiation environment. With a better understand-
ing of biological responses to space radiation, we will be able to better design our countermeasures.
Using Non-Human Organisms to Understand Radiation Damage
To fully understand the biological response of radiation in humans, NASA scientists begin the process by studying model organ-
isms. In general, biological systems are similar across many species; studying one animal can lead to deeper understandings of other
Figure 1: NASA Ames researchers in the Drosophila lab.
23 ht tp://bioastroroadmap.nasa.gov/User/risk.jsp

25
Space Faring: The Radiation Challenge
animals, even humans. Some animals are easier to study than others, and those
with short life cycles make it quicker to study multigenerational genetic eects.
Another reason these organisms are commonly used is because scientists know a
great deal about them. For most model organisms, their entire genome, physi-
ological, and behavioral characteristics are well understood. Model organisms
are small in size, so large numbers of them can be grown and studied in a small
volume, which is very important for the conned environment aboard space-
craft. Having a large population to study also reduces the statistical variation
and makes the research more accurate. Much of our understanding of life and
human disease is because of scientists’ work with model organisms. is is also
true for what is known about the biological eects of space radiation. Exam-
ples of model organisms include bacteria, yeast, worms, plants, fruit ies, and
many others. Fruit ies (g.2), like humans, have reduced ability to learn when
they are deprived of sleep. ey can also sense the direction of gravity, and are
aected by radiation. Moreover, they have many things in common with humans, including cellular processes, brain cell develop-
ment, similar behaviors, and nearly identical disease genes. In fact, there is a great deal of similarity, or homology, between the
DNA of these organisms and humans.
Other organisms like ordinary baker’s yeast (Saccharomyces cerevisiae) also contain genes for DNA repair that are very similar
to human genes with the same function. erefore we can use yeast as a model system to explore the eects of radiation on cells.
Like human cells, most yeast cells eectively repair DNA damage caused by UV radiation. However, some yeast strains have muta-
tions that prevent them from performing certain types of DNA repair. Because they cannot repair all the DNA damage, these cells
usually die after exposure to UV radiation. In addition to sensitivity to UV radiation, yeast is also sensitive to space radiation. In
a biological assessment of space radiation in low-Earth orbit, yeast inside special experiment hardware has been shown to have a
decreased rate of survival following exposure to beta particles (electrons) and low-energy protons.
24
Other ndings suggest there
are highly coordinated gene expression responses to gamma radiation. is knowledge is especially important when designing
countermeasures for astronauts during long-term lunar surface operations or microgravity spacewalks.
Plants are also commonly used in radiation studies. It has been shown that plant growth is inhibited by radiation. Like mammals,
the embryo of a plant is very sensitive to radiation damage as compared to the adult. e rate of seed germination is reduced, and
the rate of growth is slowed.
25
Excessive
UV radiation will lead to an inhibition of
plant growth processes in general. Such
alterations in primary productivity (pho-
tosynthesis) can change entire ecosystems
in the oceans, on land, and even in biore-
generative life support systems that would
be aboard future spacecraft. us, NASA
scientists must understand how plants
respond to radiation if future space explor-
ers depend upon the plants for nutrient
cycling and food. Experiments involving
plants in space, like the Biomass Production
System, have been a favorite of astronauts
during long-duration stays onboard the
International Space Station (g.3).
26
Figure 2: The fruit y is a model organism.
Figure 3: NASA scientists are looking for better ways to grow plants both on Earth and in space.
24 ht tp://mediaarchive.ksc.nasa.gov/detail.cfm?mediaid=5186
ht tp://w w w.nasa.gov/images/content/58483main_Peggy_Whitson_Plants.jpg
25 w w w.esd.ornl.gov/programs/ecorisk/documents/tm13141.pdf
26 ht tp://lifto.msfc.nasa.gov/news/2003/news-plants.asp

26
Space Faring: The Radiation Challenge
What Are the Risks and Symptoms of Radiation
Exposure for Humans?
It is important to note that the biological eects of acute and chronic radi-
ation exposure vary with the dose. An average background radiation dose
received by an average person can be approximately 3 mSv/year (including
radon) without causing detectable harm while an exposure of 1 Sv/hour
can result in radiation poisoning (nausea, vomiting). Figure 4 shows causes
of radiation exposure to the average population. A person exposed to
100 mSv has a roughly 1 in 200 chance of developing cancer later in life,
while a 1,000 mSv dose will cause cancer in about 1 in 20 people. Receiv-
ing 3,000 to 5,000 mSv during a short period of time (minutes) results in
death in 50% of the cases. A person that experiences a massive 10,000 mSv
dose will risk death in a matter of just a few days or weeks. Both acute and
chronic exposure to such large doses can cause bleeding and inammation
due to lowered platelet counts. Suppressed immune system function and
infections are possible due to lowered white blood cell counts. Reduced
fertility or permanent sterility could also result. In addition to causing
damage at the tissue, organ, and whole organism level, radiation has the ability to destroy molecules like DNA.
What Is DNA?
DNA is the blueprint of life stored in the cells of every organism. DNA contains the code for all the information required for the syn-
thesis of proteins, cell reproduction, and for organization of the tissues and organs. e information in the DNA is arranged in sections
called genes. Gene codes are read by the cell’s manufacturing system to make proteins. Proteins are the building blocks for biological
structures and for the functional machinery of the body. erefore it is vital to our health for the structure of DNA to remain intact.
What Is the Structure of DNA?
A DNA molecule (shown in g. 5) has the shape of a double helix ladder that is only ≈2 nm wide. DNA is made of individual units
called nucleotides. e information in DNA is coded in paired pyrimidine and purine nucleotides along an incredibly long mol-
ecule. A nucleotide contains three dierent types of molecules: a phosphate, a ribose sugar, and a base. e backbone of the helix is
made of alternating phosphate and ribose sugar molecules. e rungs of the ladder are base pairs. Each ribose of the backbone has
a base attached, which pairs with a base that extends from the opposite backbone. ere are four dierent types of bases in DNA:
adenine, thymine, guanine, and cytosine. DNA is arranged into 23 chromosomes in human cells. If stretched out, the DNA of one
chromosome, on average, would be about 5 cm. If all DNA in a cell were lined end to end, the molecule would reach about 3 m. If
you took all the DNA in all the cells from one human and lined it end to end, it would reach from the Earth to the sun 70 times.
Figure 4: Radioactive radon gas produced from the breakdown
of uranium in the Earth’s crust accounts for over half of the
radiation exposure to the general public.
Image Credit: University of Illinois Extension.
Cosmic
8%
Terrestrial
8%
Consumer Products
3%
Nuclear Medicine
4%
Internal
11%
Other
1%
Medical X-Rays
11%
Radon
55%
Figure 5: A drawing of DNA (left) and RNA
(right). Image Credit: The biologycorner.com.

27
Space Faring: The Radiation Challenge
What Is DNA’s Role in Protein Production?
DNA is the storage unit for the information used to make proteins. Before any protein manufacturing begins, the cell must tran-
scribe DNA into another molecule. is other “messenger” molecule will carry only the code for the specic gene to a ribosome,
which is the site of protein production. is messenger molecule is called ribonucleic acid (RNA). e ribosome reads the gene
code of a messenger RNA and manufactures proteins by assembling long chains of amino acids together, one after another, in a
process called translation. Each amino acid is coded for by a set of three nucleotides, or a codon, during translation of the RNA
message, the RNA molecule sequence is read (translated) three consecutive nucleotides at a time. A protein typically consists of
hundreds of amino acids that have been joined together. For example, imagine an RNA molecule that is 300 nucleotides long.
at RNA molecule will be decoded by a ribosome, and the ribosome will construct a protein that is a chain of exactly 100 amino
acids. A simplied chart summarizing protein production is shown in gure 6.
DNA
Transcription
RNA
Translation
Proteins
Figure 6: Protein production
What Kinds of DNA Damage Occur Due to Radiation?
DNA is normally a long, continuous molecule that stores tremendous amounts of information vital for a cell to function nor-
mally. When a DNA molecule is broken, the long chain of information is fragmented and the original message to produce specic
proteins is lost. When DNA is broken on one strand of the double helix, it is called a single strand break (SSB). If both strands
of the DNA double helix are severed within 10 to 20 base pairs of each other, the break is called a double strand break (DSB).
Figure 7 shows two examples of DNA damage. Other forms of damage that can occur include the loss of a base, and base modi-
cation such as oxidation. In many cases, cells are able to x such breaks with repair systems that are specialized for dierent types
of damage. e damage sites that remain can cause assembly of proteins to be stopped or started prematurely. If DNA replication
occurs before the repair system nds the damage, there is a chance that a modied nucleotide is misread as a dierent nucleotide.
In addition, sometimes the repair systems misread a damaged nucleotide and replace it with the wrong nucleotide. e result in
both cases is a point mutation. A point mutation is a single change in the nucleotide sequence of a gene. is can alter the amino
acid code, so that the protein produced from the gene has a dierent composition. Depending on where in the protein this occurs,
the altered protein sequence can have no aect, or it can alter the protein and protein function substantially. e result may cause
cellular or tissue abnormality. In more extreme cases, the presence of DNA damage that cannot be properly repaired can trigger
apoptosis, or cell suicide (see the next section for information about apoptosis and radiation countermeasures). e individual cell
is sacriced to prevent greater damage to the whole organism.
Figure 7: DNA model with two examples of DNA damage shown. The parallel linked sequences of orange squares () and purple circles () represent the
phosphate()-deoxyribose sugar () strands, or backbone, of a DNA molecule. The pairs of circles linking the two strands represent nucleotide base pairs.
In the single strand break, note that although some nucleotide base pairs have been separated, only one strand of the two DNA strands has been broken
(indicated by red arrow). In the more severely damaged double strand break example, nucleotide pairs have been split apart and both strands of the DNA
molecule are broken (indicated by red arrows).

28
Space Faring: The Radiation Challenge
In some cases, the eects of radiation-induced DNA damage may not be read-
ily or immediately observable. While some damage may not be severe enough to
cause death to a cell or organism, its eects can become apparent several genera-
tions later. Figure 8 is a diagram of a normal DNA molecule before and after
being hit by ionizing radiation.
27
Damage to DNA can be caused directly or indirectly. As the ion travels through
material, it will lose some of its energy to the molecules around it. Cosmic radia-
tion contains heavy ions, which are the nuclei of atoms with atomic weights
ranging from 14 (carbon) to 55 (iron) or greater. is means that the atom
is missing anywhere from 14 to 55 or more electrons. As this particle moves
through material, it will pull electrons from any source it can nd. is ionizes
the molecules along the path of the heavy ion. Protons, alpha particles, or larger
fragments can be forcibly separated from the DNA. In addition, when the heavy
ion moves through water, the hydroxide ions in water (OH-) can be ionized, los-
ing an electron, to give hydroxyl free radicals (·OH). Such species have a strong
propensity to restore the electron pair by pulling a hydrogen atom, complete with a single unpaired electron, from carbon-hydro-
gen bonds in sugars. One excellent source for this within cells is DNA. Nucleotide modications or removal, SSBs, DSBs, or any
combination of these can occur along or near the track of a heavy ion.
What Kind of Damage Can High Energy Ions Cause?
Because of their high ionization density, heavy ions and HZE particles (high energy ions, discussed in the radiation background
material) can cause clusters of damage where many molecular bonds are broken along their trajectory through the tissue. e cell’s
ability to repair DNA damage becomes impaired as the severity of clustering increases. ese particles can also create damage along
a long column of cells in tissue. In other words, cells will be damaged in streaks along the path of an HZE particle. Since HZE
particles are rare on Earth, the prediction of biological risks to humans in space must rely on fundamental knowledge gathered
from biological and medical research.
28
Because spaceight radiation biology experiments are
extremely expensive and opportunities for ight are lim-
ited, NASA models spaceight radiation exposure by
studying organisms that have been exposed to radiation
produced at special facilities here on Earth. Brookhaven
National Labs (g. 9)
29
and Lawrence Livermore National
Laboratory
30
are two examples of facilities that have the
ability to produce radiation that is similar to space radia-
tion. is type of research greatly enhances our understand-
ing of the biological response to space radiation, helps us
to anticipate what may happen during future spaceights,
and develop countermeasures to help protect astronauts
from radiation. For example, scientists have learned that
mutations, chromosomal aberrations in plant seeds, devel-
opment disturbances and malformations in small animal
embryos, and even cell death in bacteria have resulted from
the traverse of a single HZE particle.
31
Examples of cellular
damage are shown in gure 10.
Figure 8: DNA before and after ionizing radiation.
Image Credit: NASA
Figure 9: NASA Space Radiation Laboratory, at Brookhaven National Laboratory
in Upton, New York.
27 ht tp://science.nasa.gov/headlines/y2004/17feb_radiation.htm
28 ht tp://hrp.jsc.nasa.gov/?viewFile=program/srp
29 ht tp://w w w.bnl.gov/medical/NASA/NSRL_description.asp
30 ht tp://w w w.llnl.gov/
31 Acta Astronaut. 1994 Nov; 32(11):749-55.

29
Space Faring: The Radiation Challenge
This diagram
32
shows a comparison of radiation damage in three human cell nuclei (above left). The nuclei were exposed to (A) gamma rays, (B) silicon ions,
and (C) iron ions. Following exposure, the cells were stained so the scientists could observe where DNA damage occurred. Every green spot is a DSB. Notice
that the gamma ray (electromagnetic waves) exposure in (A) produced uniform damage, whereas cells exposed to high-energy heavy ions show DNA damage
along the path traveled by the ion. In (B) there is one track and in (C) there are three tracks. The damage tracks of ions with differing masses are seen in (D).
Note that heavier ions cause a wider path of destruction.
Our understanding of biological damage caused by heavy ions is very limited. A cell has been drawn
to scale for comparison purposes. Image Credit: crater.bu.edu.
What Are the Consequences of DNA Damage?
If radiation changes the number or order of nucleotides (mutation) within a DNA molecule, the information that is stored within
the DNA is altered. is can cause signicant problems in cell structures and even in their function. Even if a DNA molecule
has had only one nucleotide deleted, that error could be perpetuated when translated into RNA. In other words, when the RNA
is produced, it will be made as if that missing nucleotide had never existed in the rst place. Interestingly, the ribosome will not
know the dierence, because the cell assembles the RNA based on what it reads in the DNA. As a result, the ribosome will assume
that the information in the RNA is correct (although we know that the nucleotide order in the gene has been shifted by one nucle-
otide). Protein synthesis carries on, the triplet codons are read by the ribosome, and amino acids are gathered and assembled into a
protein structure that the DNA had not coded for originally. In this example, a malformed protein will be constructed that could
have signicant negative consequences. In summary, when the genotype (genetic information) of a cell is changed, the phenotype
(the outward observable expression of the genetic information) may also be changed. Radiation is an environmental stimuli that
has the ability to inuence whether or not a gene turns on and o, for example, some cancer genes.
32 Cucinotta, F., Lancet Oncol 2006; 7: 431–35.

30
Space Faring: The Radiation Challenge
What Is the DNA Repair System?
e repair system is constantly monitoring our DNA to make sure it stays intact; proteins will congregate to sites of damage. So one
way to measure DNA damage in tissues is by staining tissue samples to look for proteins involved in the repair system. is allows
researchers to see where the damage occurred, and at how many sites. ey can also monitor how fast the repair system takes to
complete its job by staining the tissues at dierent times after radiation exposure. When possible, cells use the unmodied comple-
mentary strand of the DNA as a template to recover the original information. Without access to a template, cells use an error-prone
recovery mechanism known as translesion synthesis as a last resort. Damage to DNA alters the three-dimensional conguration
of the helix. ese alterations can be detected by cellular repair mechanisms. Once damage is localized, specic DNA repair mol-
ecules move to the site. ese molecules bind at or near the site of damage and induce other molecules to bind and form a complex
that enables the actual repair to take place. e types of molecules involved and the mechanism of repair that assembles depend on
the type of damage that has occurred and in what phase of the cell cycle that the cell is. Some examples of specic repair systems
include: base excision repair (BER), which repairs damage due to a single nucleotide caused by oxidation, alkylation, hydrolysis, or
deamination; nucleotide excision repair (NER), which repairs damage aecting longer strands of 2-30 bases. is process recognizes
bulky, helix-distorting changes such as thymine dimers as well as SSBs; and mismatch repair (MMR), which corrects errors of DNA
replication and recombination that result in mispaired nucleotides following DNA replication.
How Does UV Radiation Affect Us?
ere are three kinds of UV radiation. UV-A radiation (wavelengths of 320-400 nm) plays a helpful and essential role in forma-
tion of Vitamin D by the skin. It is not absorbed by the ozone layer, and can cause sunburn and premature aging on human skin,
immune system problems, and cataracts in the eyes. UV-B radiation (wavelengths of 290-320 nm), mostly impacts the surface
of the skin. It is absorbed by DNA and the ozone layer, and is the primary cause of sunburn and skin cancer. After exposure to
UV-B, the skin increases production of the pigment melanin. Melanin is skin pigment found in special skin cells called Melano-
cytes. ese cells produce more melanin when exposed to UV in sunlight. e pigment absorbs the UV, preventing the UV from
aecting other parts of cells and protecting your skin from UV damage. e third is UV-C, which is completely absorbed by the
ozone layer and oxygen in the atmosphere.
DNA readily absorbs UV-B radiation as shown in gure 11. In
some cases, it causes the shape of the DNA to be changed. While
cells are able to repair this damage through the use of specialized
enzymes most of the time, sometimes damage is permanent and
the irreparable damage has a cumulative eect that is perpetu-
ated from then on as previously mentioned. UV damage can also
cause a mutation, or change in the DNA of a gene. When this
gene is transcribed and translated into a protein, the protein may
contain an error that causes it be misshapen, function improp-
erly, lead to cancer, or even cause cells to kill themselves.
33
One in ve Americans will develop skin cancer and one Ameri-
can dies from this disease every hour. People who have had
several blistering sunburns before age 18 are at higher risk of
developing melanoma, the most serious form of skin cancer.
Individuals with fair skin and freckles have a higher risk of
developing skin cancer, but dark-skinned individuals can also
get this cancer. Regardless of your skin color, exposure to UV
radiation can lead to premature aging of the skin, causing it to become thick, wrinkled, and leathery. Proteins in the lens of the eye
can also be altered by radiation, leading to the formation of cataracts that can lead to partial or complete blindness. UV radiation
may also suppress proper functioning of the body’s immune system.
Figure 11: DNA readily absorbs UV-B radiation.
33 ht tp://earthobservatory.nasa.gov/Library/UVB/

31
Space Faring: The Radiation Challenge
How Do Sunscreens Work?
Sunscreens act like a very thin shield by stopping the UV radiation before it can enter the skin and cause damage. Some sunscreens
contain organic molecules (such as oxybenzone, homosalate, and PABA) that absorb UV-B and/or UV-A radiation. Others use
inorganic pigments (such as titanium dioxide and zinc oxide or both) that absorb, scatter, and reect both UV-A and UV-B light.
Sunscreens are labeled with a Sun Protection Factor (SPF) rating that could also be thought of as a sunburn protection factor. For
example, suppose that your skin begins to redden after 10 minutes in the sun. If you protected it with an SPF 15 sunscreen, it
would take 15 times as long, or 2.5 hours, to get a comparable burn. Remember, SPF relates only to UVB protection; there is no
standard measurement or rating for UV-A protection in the United States.
What Is Degenerative Tissue Damage?
As we have discussed, ionizing radiation alters DNA such that cell repair processes, cell cycle, or cell division are aected. Low
numbers of SSB or DSB may provide a trigger for the gradual loss of cycling cells. Loss of repair mechanisms, or loss or reduction
of cell division results in tissue degeneration. is can occur in almost all tissues, including the nervous system.
ere are also radiation-induced bystander eects. ese are biological responses in cells that are not themselves directly in the
path of ionizing radiation or in a eld of radiation. In fact, new studies show that an even larger portion of bystander cells, some-
times at considerable distance from the irradiated cells, can be aected. e radiation eects can be transmitted directly from
cell to cell through channels (gap junctions) connecting cells. Alternatively, a directly hit cell can secrete factors, or signals, which
travel out of the hit cell to neighboring cells. Bystander eects have been clearly established in cell culture systems, and a few stud-
ies are starting to provide evidence that bystander eects occur in vivo (the natural setting). Bystander eects amplify or exaggerate
the action of even low dose radiation, so they can signicantly increase radiation risk and tissue damage. is may be particularly
important when ionizing radiation hits the nervous system, where bystander eects could lead to loss of sensory, motor, and cogni-
tive functions.
34
Degenerative tissue damage and central nervous system dam-
age could be particularly dangerous if it occurs in the brain (see
g. 12) of astronauts. e damage could cause altered behavior.
Since damage to the nervous system is not repairable, it could
reduce the ability of astronauts to work and respond to their
environment, especially in an emergency. It could eventually
lead to loss of control over their entire body, or death.
Figure 12: In this image, brain necrosis (unprogrammed cell death) has
occurred. Similar damage could result from excessive radiation.
34 Boyle, R., Radiation Biology Professional Development Course Charts, 2006.

32
Space Faring: The Radiation Challenge
Activity II: Modeling Radiation-Damaged DNA
In Activity II, students will use candy (or Styrofoam balls) to construct a model of deoxyribonucleic acid (DNA) and will then
alter the model to visualize what happens to DNA when it is damaged by radiation.
You can customize this activity by instructing the students to either: (1) Construct a DNA model by rst building individual
nucleotides, and then assembling the double-stranded DNA molecule (page 4; this more accurately represents the natural bio-
chemical process of DNA assembly), or (2) Construct the entire DNA model exactly as shown in the activity (page 5).
Background
DNA is the blueprint of life stored in the cells of every organism. A DNA mol-
ecule has the shape of a double helix ladder that is only ≈2 nm wide. DNA is
made of individual units called nucleotides. Each nucleotide has two parts – a
phosphate-sugar part that forms part of the backbone, or strand, and the base
that is the information for the sequence, or, genetic code. e backbone strands
of the helix are made of alternating phosphate and ribose sugar molecules. e
bases match up along the center of the ladder to join the two strands together.
e base pairs form the “rungs” of the DNA ladder. ere are just four dier-
ent types of bases in DNA: adenine, thymine, guanine, and cytosine. Figure 13
shows computer-generated molecular models of normal DNA, and DNA that
is experiencing damage due to incoming radiation. Breaks in the two strands
that form the backbone of DNA are among the most dicult for cells to repair.
Radiation can sever one or both strands of the molecule, forming single or
double strand breaks. Figure 14 is a diagram showing the dierence between
the two forms of damage on an DNA molecule. In this activity, students will
start by building 4-base-pair models of a DNA molecule, and then they will
join together in groups of four to combine the 4-base-pair models together and
create a 16-base-pair DNA model. Refer to Modules 1 and 2 for background
information about radiation and biological eects of radiation exposure.
Figure 13: Molecular model depicting normal DNA (left)
and radiation damaged DNA (right). Image Credit: NASA

33
Space Faring: The Radiation Challenge
Figure 14. DNA model with two examples of DNA damage shown. The parallel linked sequences of orange squares () and purple circles () represent the
phosphate()-deoxyribose sugar () strands, or backbone, of a DNA molecule. The pairs of circles linking the two strands represent nucleotide base pairs.
In the single strand break, note that although some nucleotide base pairs have been separated, only one strand of the two DNA strands has been broken
(indicated by red arrow). In the more severely damaged double strand break example, nucleotide pairs have been split apart and both strands of the DNA
molecule are broken (indicated by red arrows).
Objectives:
By the end of this lesson, the students will be able to:
• Construct a model of a DNA molecule.
• Understand that DNA can be damaged from radiation.
• Visualize models of dierent kinds of radiation-damaged DNA.
• Explain the dierence between double strand and single strand breaks.
Research Question:
Why is a double strand break in DNA more damaging than a single strand break?
Discussion Questions:
For planning a human-tended lunar outpost, have students discuss in detail how the presence of space radiation will aect the
design of habitats for humans and other living organisms (such as crops grown for food). Other possible topics for discussion
include:
• How many strands make up DNA?
• What does DNA do?
• What is a single strand break?
• What is a double strand break?
• Can DNA function when it is broken?
• What do the toothpicks in this activity represent?
• What kinds of radiation can damage DNA?
National Education Standards
35
:
Unifying Concepts and Processes
Systems, order and organization
Evidence, models, and explanation
Science in Personal and Social Perspectives
Natural hazards
Personal health
35 National Science Education Standards, Center for Science, Mathematics, and Engineering Education (CSMEE), National Academy of Sciences, National
Academy Press, Washington, DC., 1996, ISBN 0-309-05326-9.

34
Space Faring: The Radiation Challenge
Science and technology in society
Physical Science
Transfer of Energy
Earth and Space Science
Structure of the Earth system
Materials:
1. Gum drops, ve colors minimum (As an alternative, marshmallows could be used).
2. Candy orange slices, (or other soft candy that is larger than gum drops).
3. Plain at toothpicks (may be cut in half).
4. Option: One inch-diameter Styrofoam balls can be substituted for candy. e balls can be colored or labeled by the students
to represent the bases, phosphates and sugars. ere should be a minimum of 6 dierent colored items.
5. Colored pencils
6. 4 – 5 Paper towels each, or a large piece of paper, to provide working space
7. Large table (or space on oor) to place long DNA models
Provide each student with the candies (or Styrofoam balls) and toothpicks needed to construct a DNA molecule that is four base
pairs in length. Dene the key for your models below.
Number of candies for each DNA Model: (ll in color)
8 = (P)
_________________ = Phosphate group
8 = (Sugar)
_____________ = Deoxyribose sugar group
2 = (C)
_________________ = Cytosine base
2 = (G)
_________________ = Guanine base
2 = (T)
_________________ = Thymine base
2 = (A)
_________________ = Adenine base
30 = (lines) Toothpicks = chemical bonds
After each student has constructed their model, partner four students together and combine all four models to create one 16-base-
pair long DNA model.
Time allotment: 60 - 120 minutes
References:
Additional three-dimensional DNA modeling can be done using kits that are available commercially from science education
material suppliers.
Going Further:
For additional research opportunities, have students investigate:
• Astrobiology and Radiation (to understand the eect of radiation on the surface of Mars and implications for life on Mars).
• Benecial uses of radiation, such as radiation therapy, nuclear imaging in medicine (CT Scans or PET Scans),
• Brachytherapy, or the use of radioactive material in smoke detectors.

35
Space Faring: The Radiation Challenge
Name: _____________________________________ Date: ________________________
Constructing A DNA Model One Nucleotide At A Time
Directions: Use the instructions and diagrams below to help construct your model of DNA. e model that you will create will
be made from eight nucleotides. e nucleotides will be assembled together to create a DNA model that is four complimentary
nucleotide pairs in length - the completed model will look like a ladder. After lling in the color key to distinguish each compo-
nent in the DNA model, use toothpicks to connect the candies together as shown in the diagram below. Each toothpick represents
the chemical bonds that hold the building blocks of DNA together.
1. Working on a clean surface, group candies by color. Determine which color will represent each DNA component and ll in the
key. en color or write in the color name in the diagram below showing the P, Sugar, C, G, A, and T.
Key for DNA Model (ll color in blank):
(P)
= Phosphate group = _____________________
(Sugar) = Deoxyribose sugar group = ____________
(C) = Cytosine base = ________________________
(G) = Guanine base = ________________________
(T) = Thymine base = ________________________
(A) = Adenine base = ________________________
(lines) Toothpicks = chemical bonds
2. Construct the four nucleotides as shown in the diagram below.
3. To construct the rst strand of DNA, place each nucleotide laying at on the table in front of you. Use a toothpick to connect
the sugar of one nucleotide with the phosphate of another. Repeat this step until all four nucleotides are connected. When this
is complete, one strand of your DNA molecule is nished.

36
Space Faring: The Radiation Challenge
4. Construct four more nucleotides identical to those you just constructed.
5. Connect the correct complimentary base to your rst nucleotide to form the rst base pairing in the DNA “ladder”. Remem-
ber: in DNA, adenine only bonds with thymine (A:T or T:A), and cytosine only bonds with guanine (C:G or G:C), and the
phosphate group links the deoxyribose sugars to form the backbone. If you need help, use the diagram in the discussion sheet.
6. Continue adding the remaining nucleotides to form your DNA model. When all eight nucleotides are in place, you have com-
pleted your double-stranded model of DNA.
7. Follow the instructions and answer the questions on the “Modeling Radiation Damaged DNA Discussion Sheet.”

37
Space Faring: The Radiation Challenge
Name: _____________________________________ Date: ________________________
Constructing A DNA Model
Directions: Use the diagram below to help construct your model of DNA. is will vary depending upon your model compo-
nents. e color key identies each component of the DNA model. Use toothpicks to connect the candies (or Styrofoam balls)
together. e toothpick connections represent the chemical bonds that hold the building blocks of the DNA molecule together.
After follow the instructions and building your DNA molecule, answer the questions on the “Modeling Radiation-Damaged DNA
Discussion Sheet.”
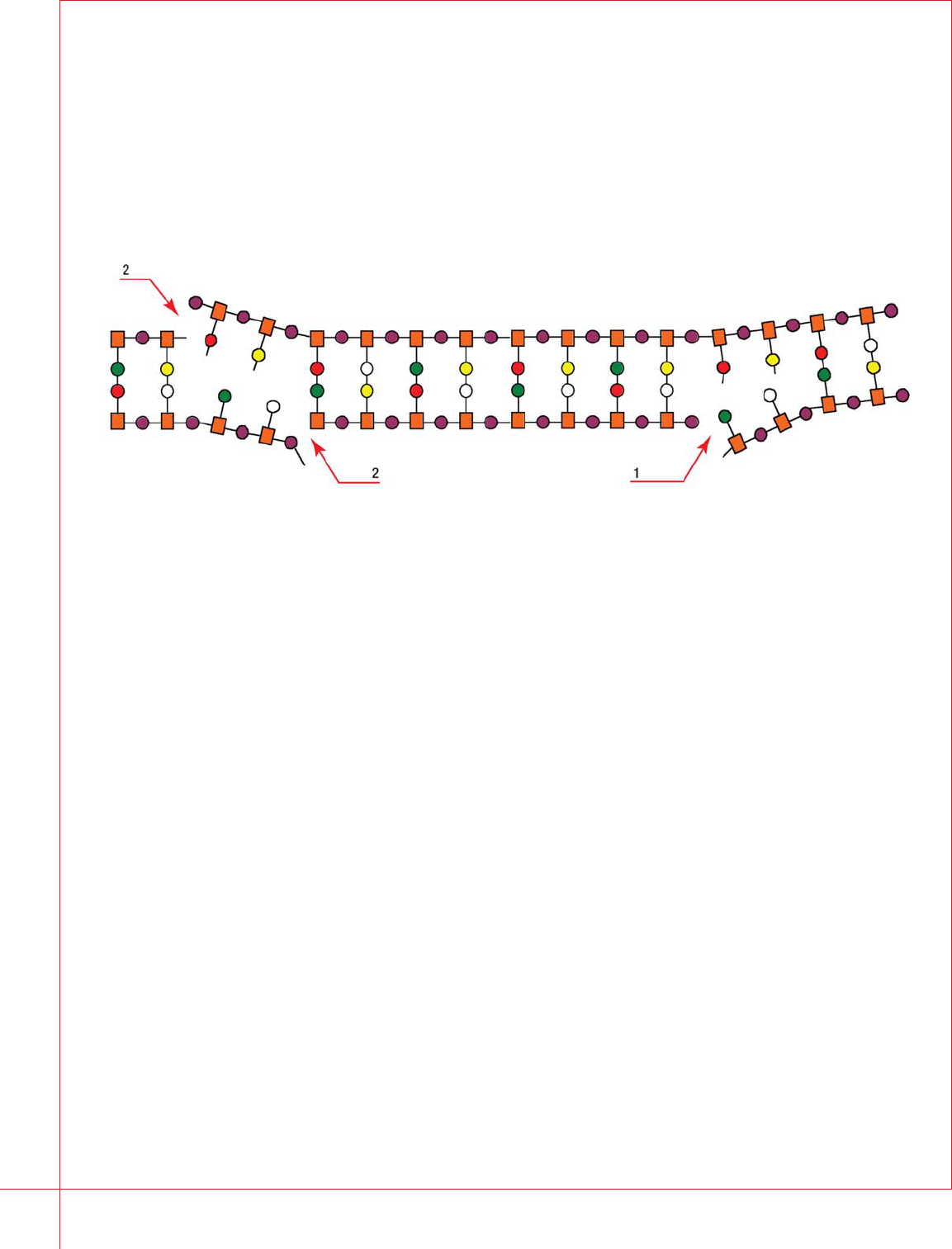
38
Space Faring: The Radiation Challenge
Name: _____________________________________ Date: ________________________
Modeling Radiation Damaged DNA Discussion Sheet
(1) How many strands of nucleotides make up DNA?
(2) Study the diagram below. Partner up with three other students and combine your models to make a longer DNA model.
Imagine that your DNA molecule is being bombarded by radiation. Modify your DNA model to look similar to the break
labeled “1.” Answer the following questions:
How many nucleotide strands of your DNA model have been broken? _________
What do the toothpicks represent? _____________________________________
Is your DNA model in one or two pieces? ____________
Is this a single or double strand break? ______________
(3) Imagine that even more radiation bombards your DNA molecule. Modify your DNA model to look similar to the break
labeled “2.” Answer the following questions:
How many nucleotide strands of your DNA model have been broken? _________
Is your DNA model in one or two pieces? ____________
Is this a single or double strand break? ______________
(4) Which chemical bonds must be repaired in a double strand break to return the molecule back to its original shape?
(5) Can DNA function normally if it is broken?

39
Space Faring: The Radiation Challenge
(6) What eect would a few single strand breaks would have on a cell? On the body?
(7) What eect would many double strand breaks would have on a cell? On the body?
(8) What kinds of radiation can damage DNA?

40
Space Faring: The Radiation Challenge
Answer Key Modeling Radiation Damaged DNA Discussion Sheet
(1) How many strands of nucleotides make up DNA?
two
(2) Study the diagram below. Partner up with three other students and combine your models to make a longer DNA model.
Imagine that your DNA molecule is being bombarded by radiation. Modify your DNA model to look similar to the break
labeled “1.” Answer the following questions:
How many nucleotide strands of your DNA model have been broken? one
What do the toothpicks represent? chemical bonds that hold the building blocks of the DNA molecule together
Is your DNA model in one or two pieces? one
Is this a single or double strand break? single strand break
(3) Imagine that even more radiation bombards your DNA molecule. Modify your DNA model to look similar to the break
labeled “2.” Answer the following questions:
How many nucleotide strands of your DNA model have been broken? two
Is your DNA model in one or two pieces? two
Is this a single or double strand break? double strand break
(4) Which chemical bonds must be repaired in a double strand break to return the molecule back to its original shape?
e bonds between the phosphates and sugars on both DNA strands, and those between the nucleotides must be repaired.
(5) Can DNA function normally if it is broken?
No, not until it is repaired.
(6) What eect would a few single strand breaks would have on a cell? On the body?
Cells with DNA containing a few sites of single stranded damage are likely to be able to repair the damage. However, some of
repair may be done incorrectly. Incorrectly repaired DNA can result in mutations within the genetic code. Dependingon the region
of DNA where a mutation takes place, the result may have no physiological consequence, or it may cause minor or major changes
in how a cell functions. One or more mutations can reduce the ability of a cell to control cell division. If this happens, the exposed
person may develop cancer. ese eects may take years to decades to become apparent.

41
Space Faring: The Radiation Challenge
(7) What eect would many double strand breaks would have on a cell? On the body?
Many double strand breaks would badly damage DNA. is would be dicult for a cell to repair. Cells that contain DNA that
is badly damaged may not be able to repair the damage, and the cells die. If this occurs in only a few cells, this is actually better for
the organism, because there is then no chance of mutations resulting from faulty repair of the DNA. However, if DNA is badly
damaged in many cells in a particular tissue or organ, and a large number of cells die, then that tissue or organ no longer can
function properly. is can compromise the exposed person’s health, within weeks, or over time, up to years.
(8) What kinds of radiation can damage DNA?
High energy, ionizing radiation such as X-rays and gamma rays, and particle radiation such as galactic cosmic radiation.

42
Space Faring: The Radiation Challenge
Protection from Radiation
Space radiation can penetrate habitats, spacecraft, equipment, spacesuits, and can harm astronauts.
Minimizing the physiological changes caused by space radiation exposure is one of the biggest chal-
lenges in keeping astronauts t and healthy as they travel through the solar system. As mentioned
previously, ionizing radiation is a serious problem that can cause damage to all parts of the body
including the central nervous system, skin, gastrointestinal tract, skeletal system, and the blood form-
ing organs. However, biological damage due to radiation can be mitigated through implementation of
countermeasures that are designed to reduce radiation exposure and its eects. In this section, we will
discuss the use of radiation dosimetry and operational, engineering, and dietary countermeasures.
Why is NASA Studying Radiation Countermeasures?
Radiation protection is essential for humans to live and work safely in space. To accomplish this challenging task, NASA has devel-
oped the Radiation Health Program. e goal of the program is to carry out the human exploration and development of space
without exceeding acceptable risk from exposure to ionizing radiation. Legal, moral, and practical considerations require that
NASA limit risks incurred by humans living and working in space to acceptable levels.
36
To determine acceptable levels of risk for
astronauts, NASA follows the standard radiation protection practices recommended by the U.S. National Academy of Sciences
Space Science Board and the U.S. National Council on Radiation Protection and Measurements.
37
What is Radiation Dosimetry?
In low Earth orbit, astronauts lose the natural shielding from solar and cosmic radiation
provided by the Earth’s atmosphere. In deep space astronauts also lose the shielding pro-
vided by the Earth’s strong magnetic eld. So, to achieve the goal of the NASA Radiation
Health Program, it is necessary to monitor the radiation environment inside and outside
a manned spacecraft.
An important part of every manned mission is radiation dosimetry, which is the process of
monitoring, characterizing, and quantifying the radiation environment where astronauts
live and work. Radiation biology support during missions also includes: calculated esti-
mates of crew exposure during extra-vehicular activity; evaluation of any radiation-produc-
ing equipment carried on the spacecraft; and comprehensive computer modeling of crew
exposure. Space station crewmembers routinely wear physical dosimeters to measure their
accumulated exposure and, post ight, provide a blood sample to measure radiation dam-
age to chromosomes in blood cells.
38
In addition, experiments on the Space Station have
been carried out using a synthetic human torso, which has over 300 strategically placed
dosimeters to determine the levels of cosmic radiation absorbed by specic organs in the
human body during space ight.
39
Active monitoring of space radiation levels within the
Space Station is achieved with dosimeters both to identify the best-shielded locations
within the Space Station and to give early warning should radiation levels increase during
a mission due to solar storms.
All these sources of information are carefully analyzed before, during, and after to help mission planners mitigate the four signi-
cant radiation-related health risks that are described in the NASA Bioastronautics Critical Path Roadmap:
40
cancer, radiation dam-
age to the central nervous system, chronic and degenerative tissue diseases, and acute radiation sickness. See the previous section
for information on the biological eects of radiation.
NASA uses an anatomical model of a
human torso and head that contains more
than 300 radiation sensors.
36 ht tp://srag.jsc.nasa.gov/Index.cfm#
37 ht tp://w w w.nasa.gov/audience/foreducators/postsecondary/features/F_Understanding_Space_Radiation_prt.htm
38 ht tp://exploration.nasa.gov/programs/station/Chromosome-2.html
39 ht tp://exploration.nasa.gov/programs/station/Torso.html
40 ht tp://bioastroroadmap.nasa.gov/User/risk.jsp

43
Space Faring: The Radiation Challenge
What Are Operational Countermeasures?
Currently, the main operational countermeasure against the adverse aects of radiation is simply limiting astronaut exposure,
which means limiting the amount of time astronauts are allowed to be in space. is is accomplished primarily by shortening
overall mission duration on the Space Station to 3-6 months, reducing the time astronauts spend outside of the spacecraft during
spacewalks, and planning space missions during times of reduced solar storm activity. However, since future long-term missions of
exploration to the Moon and beyond will both take longer (a round-trip to Mars will last at least two years) and expose astronauts
to a more damaging types of radiation, other strategies such as better shielding and mitigation strategies are necessary before astro-
nauts can spend extended periods in deep space.
What Are Engineering Countermeasures?
Engineering countermeasures are structures or tools that are designed to shield astronauts
from radiation. Depending on where astronauts are living and working, the radiation
shielding requirements will vary because of exposure to dierent types and levels of radia-
tion. e most penetrating ionizing radiation (gamma rays and galactic cosmic rays) can
pass through aluminum but is stopped by thick and dense material such as cement. In
general, the best shields will be able to block a spectrum of radiation. Aboard the space
station, the use of hydrogen-rich shielding such as polyethylene in the most frequently
occupied locations, such as the sleeping quarters and the galley, has reduced the crew’s
exposure to space radiation. Since the Space Shuttle and the International Space Station
are in low Earth orbit, where the quantity and energy of the radiation is lower and the
Earth’s atmosphere provides protection, these spacecraft require less shielding than a base
on the surface of the Moon. On the Moon, radiation shields would need to be very thick
to prevent the primary cosmic rays (high-energy protons and heavy ions) from penetrating
into habitation modules where astronauts will live. Such shielding could include the metal
shell of a spacecraft or habitation module, an insulating layer of lunar water, or both.
Problems with shields arise when space radiation particles interact with the atoms of the shield
itself. ese interactions lead to production of nuclear byproducts called secondaries (neu-
trons and other particles). If the shield isn’t thick enough to contain them, the secondaries
that enter the spacecraft can be worse for astronauts’ health than the primary space radiation.
Surprisingly, heavier elements such as lead produce more secondary radiation than lighter
elements such as carbon and hydrogen. Consequently, a great deal of research has been per-
formed on a lightweight polyethylene plastic, called RFX1, which is composed entirely of
lightweight carbon and hydrogen atoms.
41
Research shows that polyethylene is 50% better at
shielding solar ares and is 15% better at shielding galactic cosmic radiation as compared to
aluminum. Water is another hydrogen-rich molecule that can absorb radiation. However, the
oxygen content in water makes it a lot heavier than polyethylene, and therefore is much more
expensive to launch. Generally, lighter shields can greatly reduce the harmful eects of incom-
ing space radiation particles, but they cannot completely stop them.
NASA scientists have also investigated the development of electrostatic radiation shields,
42
which generate positive and negative
electric charges that deect incoming electrically charged space radiation. Another method of radiation protection that has been
proposed is to use the lunar regolith (the pulverized dusty material on the Moon’s surface) to shield a human colony.
The composition and thickness of a
material affects its ability to shield radiation.
Collisions between high-energy
radiation and shielding can produce
damaging secondary particles.
41 ht tp://science.nasa.gov/headlines/y2005/25aug_plasticspaceships.htm
42 ht tp://w w w.nasa.gov/centers/goddard/news/topstory/2004/0930grb.html

44
Space Faring: The Radiation Challenge
Although existing shielding can solve some radiation con-
cerns, it makes spacecraft heavy and expensive to launch.
Moreover, it does not provide complete protection against
radiation. Shields ve to seven centimeters thick can only
block 30 to 35 percent of the radiation, which means that
astronauts could still be exposed to up to 70 percent of the
radiation that passes through the shields.
43
For this reason,
NASA is also investigating the use of medical and dietary sup-
plements to mitigate the eects of ionizing radiation.
NASA has investigated electrostatic and plastic shielding. Combinations of
different engineering, operational, and dietary countermeasuers help improve
radiation protection. Image Credit: NASA Goddard Space Flight Center.
What are Dietary Countermeasures?
Dietary countermeasures are drugs, that when ingested by
an astronaut, may have the potential to reduce eects of
ionizing radiation. ese supplements can be broadly cat-
egorized into two groups. e rst group includes specic
nutrients that prevent the radiation damage. For example,
antioxidants like vitamins C and A may help by soaking
up radiation-produced free-radicals before they can do any
harm. Research has also suggested that pectin ber from
fruits and vegetables, and omega-3-rich sh oils may be
benecial countermeasures to damage from long-term radia-
tion exposure. Other studies have shown that diets rich in
strawberries, blueberries, kale and spinach prevent neuro-
logical damage due to radiation. In addition, drugs such as
Radiogardase (also known as Prussian blue) that contain
Ferric (III) hexacyanoferrate (II) are designed to increase the
rate at which radioactive substances like cesium-137 or thal-
lium are eliminated from the body.
44
e second group of dietary agents currently being con-
sidered for protection against ionizing radiation includes
drugs that can facilitate faster recovery from radiation dam-
age. ese dietary agents oer protection by stimulating the
growth of surviving stem and progenitor cells, or by length-
ening the duration of the cell cycle segment that checks for and repairs damaged genes.
45
Although these types of drugs (radiopro-
tectants) are now used to treat people exposed to radiation contamination on Earth, they may be good candidates for use on long
duration space missions. It is important to note, however, that when administered in eective concentrations, some radioprotectants
also have limiting negative side eects such as nausea, hypotension, weakness, and fatigue.
One natural defense system is for an abnormal radiation damaged cell to self-destruct before the cell becomes cancerous; this is
achieved by activation of the cell’s apoptosis gene (programmed cell death). Apoptosis can also be triggered intentionally by exposing
the cell to enzymes or specic ligands that bind to a cell’s death receptors. Other approaches that may also be useful aim to enhance
the DNA repair system and immunoresponse by facilitating faster recovery of cell populations damaged by radiation. ere are
several such pharmaceuticals now in clinical trials. Some drugs, for example, stimulate the immune system to “restore and repopu-
late” bone marrow cells after radiation exposure. Other drugs appear to reduce gene mutations resulting from radiation exposure.
Thymus
T Lymphocyte
NK Lymphocyte
B Lymphocyte
Erythrocyte
Megakaryocyte
(blood clotting)
Macrophage
Granulocyte
Monocyte
Plasma Cell
Pluriport
Stem Cell
Stem cells in the bone marrow produce a wide range of blood cell types.
Image Credit: Stem Cell World.
43 ht tp://w w w.nasa.gov/vision/space/travelinginspace/keeping_astronauts_healthy_prt.htm
44 ht tp://w w w.fda.gov/bbs/topics/NEWS/2003/NEW00950.html
45 ht tp://w w w.nasa.gov/vision/space/travelinginspace/keeping_astronauts_healthy_prt.htm

45
Space Faring: The Radiation Challenge
Radiation protectants originally developed to protect military personnel in
the event of nuclear warfare are now being used to protect cancer patients
against the harmful eects of radiation treatment. Although large doses of
ionizing radiation are damaging, small amounts are required for some bio-
logical processes. For example, vitamin D, necessary for maintenance and
growth of bones, is normally produced in a person’s skin through exposure
to ultraviolet light. Since the Space Station is shielded to keep out harmful
amounts of ultraviolet radiation, normal vitamin D production in an astro-
naut’s skin is inhibited. To compensate, the astronauts will require vitamin
D supplements.
46
Dietary countermeasures have effects at the molecular level.
Image Credit: NASA.
46 ht tp://w w w.nasa.gov/vision/space/travelinginspace/keeping_astronauts_healthy_prt.htm

46
Space Faring: The Radiation Challenge
Activity III: Space Weather Forecasting
In Activity III, students will investigate solar activity by plotting sun spot data (from 1945 to present) and by interpreting images
of the sun. e students will use the data to predict the best time for future long duration human spaceight missions to Mars.
e data can be graphed by hand on graph paper or with a computer. Alternatively, you can provide them the graph found at the
end of this activity.
Background
To help students understand space weather and how it inuences spaceight mission planning, we can use the analogy of traveling
by car during winter months here on Earth. For example, if you knew that cold weather or even a blizzard were possible during a
trip, you would prepare for such conditions by packing a winter survival kit, blankets, warm clothing, food, and other gear neces-
sary to survive in the storm in the event something would go wrong. However, if you were able to read a weather forecast before
embarking on your trip, you might nd that you could leave a few days early or a few days later to avoid the cold, blizzard-like
conditions entirely. Like a winter weather forecast, we can use space weather forecasts to help plan for spaceight missions and
reduce dangers and problems associated with radiation while exploring space.
The Solar Cycle
For hundreds of years, scientists have been studying the Sun and have noticed that it has an 11-year cycle of sunspot activity.
47
During “solar maximum,” the Sun is very active, has a large number of sunspots, and eectively shields the inner solar system from
most galactic cosmic rays (GCRs).
48
During “solar minimum,” the Sun is relatively inactive, has a low number of sunspots, and
subsequently allows GCRs to reach the inner solar system in greater numbers.
e dose from GCRs is approximately 2.5 times
higher at solar minimum than at solar maximum.
49
It is also important to note that some solar activity that aects the radiation environment of the solar system cannot be predicted
with the same accuracy as sunspots. In addition to electromagnetic radiation, the Sun sometimes emits huge streams of particle
radiation during events called Coronal Mass Ejections (CMEs). A CME is when the sun sprays a fountain of plasma that consists
mainly of electrons, protons, and other elements like helium, oxygen, and iron away from the solar surface. CMEs vary in size;
they can be much larger than the Earth. Coronal Mass Ejections occur more frequently during solar maximum, and can be harm-
ful to astronauts. Particle radiation from a Coronal Mass Ejection can travel at varying speeds. e average speeds are about 424
km/s, and will reach the Earth or the Earth’s Moon in about 98 hours, or Mars in 150 hours (assuming that Mars is 228,000,000
km away from the Sun).
50
CMEs are a particularly high risk event for astronauts because of our inability to predict them. ey occur about once every
month during solar maximum and once every eight months during solar minimum. During a trip to Mars, it is highly likely that
astronauts might encounter three or more CMEs, and probably more while on the surface of Mars, depending upon the duration
of their stay.
51
It has been estimated that if a major CME occurred while astronauts were on the Moon, their skin could receive an
acute radiation dose up to 6 Sv, with bone marrow doses close to 0.9 Sv, which might cause some health problems (see the health
eects from acute radiation exposure in Activity 2).
In summary, the information we know and gather about sunspots allows scientists to predict when the sun will be most active
and when it will be least active, which in turn allows us to determine when the radiation environment of the solar system will be
potentially less harmful for astronaut explorers. We can develop space weather forecasts that can be used to help in planning when
47 ht tp://sohow w w.nascom.nasa.gov/classroom/classroom.html
48 GCRs are a form of very high-energy particle radiation that come from outside the solar system and can be damaging to spacecraft and astronauts. For more
information on GCRs, see Module 1 and 2 of the Radiation Biology Educator Guide.
49 ht tp://image.gsfc.nasa.gov/poetry/workbook/p72.html
50 ht tp://sohow w w.nascom.nasa.gov/classroom/notsofaq.html#CME_SPEED
51 ht tp://image.gsfc.nasa.gov/poetry/workbook/p74.html

47
Space Faring: The Radiation Challenge
a mission should take place. e forecast can also be used to identify periods of time when astronauts and sensitive electronics or
hardware might need more protection from harmful blasts of solar radiation.
Objectives:
By the end of this lesson, the students will be able to:
• Identify sunspots in images of the Sun.
• Plot sunspot number versus time on a graph (this chart could be provided to students if they are unable to plot the data).
• Understand a graph of sunspot data.
• Understand that scientists have observed sunspots for hundreds of years.
• Describe how the number of sunspots on the Sun changes over time.
• Describe how solar activity can be used in spaceight mission planning.
• Explain why protecting people and astronauts from radiation is important.
Research Question:
In what years will the next solar maximum and solar minimum occur, and which is best for astronaut travel?
Discussion Questions:
Have students discuss in detail how solar weather inuences the distance astronauts could travel away from the protective shelter
of a lunar outpost. Other possible topics for discussion include:
• When is the next solar maximum? e next solar minimum?
• Why must astronauts be shielded from radiation?
• How can solar activity data be used in space weather forecasting?
• What is the duration of the solar cycle?
• How long does it take a Coronal Mass Ejection to reach Earth? Mars?
National Education Standards
52
:
Unifying Concepts and Processes
Evidence, models, and explanation
Change, constancy, and measurement
Form and function
Science as Inquiry
Abilities necessary to do scientic inquiry
Understandings about scientic inquiry
Physical Science
Properties and changes of properties in matter
Life Science
Diversity and adaptations of organisms
Earth and Space Science
Earth in the solar system
Science in Personal and Social Perspectives
Risks and Benets
Natural Hazards
52 National Science Education Standards, Center for Science, Mathematics, and Engineering Education (CSMEE), National Academy of Sciences, National
Academy Press, Washington, DC., 1996, ISBN 0-309-05326-9.

48
Space Faring: The Radiation Challenge
Materials:
After describing to the students the dierence between solar maximum and solar minimum, provide the students the Sunspot
Data Set, the Sunspot Worksheet, and the Space Weather Forecasting Worksheet, the glossary, and the following materials:
1. Graph paper
2. Colored pencils (red and green, other colors may also be used)
3. Optional: Computer with graphing capability
4. Optional: the completed graph of sunspot activity
Time allotment: 60-90 minutes
References:
ht tp://w w w.spaceweather.com/
ht tp://sohow w w.nascom.nasa.gov/
ht tp://science.msfc.nasa.gov/ssl/pad/solar/images/zurich.gif
Going Further:
For additional research opportunities, have students investigate:
• Solar activity
• e SOHO spacecraft
• Space weather on the Moon and Mars
• e Maunder Minimum
• e history of sunspot observations

49
Space Faring: The Radiation Challenge
Sunspot Data Set
Directions: Use this data set to graph the number of sunspots that occurred from 1945 to 2005.
53
Plot the year on the x-axis and
the number of sunspots on the y-axis using the Plotting Sunspots on a Graph Worksheet or a computer. Connect the dots to see
the trends in sunspots. Answer the questions on the Space Weather Forecasting Worksheet and Sunspot Worksheet.
Sunspots Per Year
Year
Number of Sunspots
(average)
Year
Number of Sunspots
(average)
1945 32 1976 12
1946 100 1977 26
1947 171 1978 87
1948 167 1979 146
1949 174 1980 149
1950 104 1981 147
1951 64 1982 115
1952 31 1983 65
1953 13 1984 44
1954 3 1985 16
1955 35 1986 11
1956 126 1987 29
1957 168 1988 101
1958 172 1989 162
1959 145 1990 145
1960 102 1991 144
1961 45 1992 94
1962 30 1993 55
1963 22 1994 31
1964 7 1995 18
1965 12 1996 8
1966 39 1997 20
1967 86 1998 62
1968 98 1999 96
1969 105 2000 123
1970 107 2001 123
1971 67 2002 109
1972 67 2003 66
1973 37 2004 43
1974 32 2005 30
1975 14 2006 15
53 ftp://ftp.ngdc.noaa.gov/STP/SOLAR_DATA/SUNSPOT_NUMBERS/AMERICAN_NUMBERS/YEARLY is data has been rounded to the nearest whole
number. An observer computes a daily sunspot number by multiplying the number of groups he/she sees by ten and then adding this product to his total
count of individual spots. Results, however, vary greatly, since the measurement strongly depends on observer interpretation and experience and on the stabil-
ity of the Earth’s atmosphere above the observing site. Moreover, the use of Earth as a platform from which to record these numbers contributes to their vari-
ability, too, because the sun rotates and the evolving spot groups are distributed unevenly across solar longitudes. To compensate for these limitations, each
daily international number is computed as a weighted average of measurements made from a network of cooperating observatories.

50
Space Faring: The Radiation Challenge
Name: _____________________________________ Date: ________________________
Sunspot Worksheet
Directions: Answer the questions by studying the images of the sun.
Image Credit: NASA Solar and Heliospheric Observatory (SOHO).
(1) Observe the two images of the sun. Describe how the images dier.
(2) How many sunspots can you count in the left image? ________________
(3) How many sunspots are in the right image? ________________
(4) In which picture does the sun seem more active? Why?
(5) Which solar condition would you predict is better for reducing Galactic Cosmic Radiation exposure to astronauts during long
duration space travel?

51
Space Faring: The Radiation Challenge
Name: _____________________________________ Date: ________________________
Space Weather Forecasting Worksheet
Directions: Answer the following questions by using your graph of sun spot data and the sunspot worksheet.
(1) In what year did the most number of sunspots occur? _______________
(2) In what year did the least number of sunspots occur? ________________
(3) On average, how many years are between the peak sunspot activity? ______________
(is period of time is known as the solar cycle).
(4) Does the sun vary in its activity? ______________ Why?
(5) Where might the left image from page 1 of the worksheet be located on this graph? Mark the position the graph with a green “O”.
(6) Where might the right image from page 1 of the worksheet be located on this graph? Mark the position on the graph with a
red “X.”
(7) Approximately what year will be the next solar maximum? _______________
Will this be a good travel time for astronauts?________________ Why or why not?
(8) Approximately what year will be the next solar minimum? _______________
Will this be a good travel time for astronauts? ________________ Why or why not?
(9) If you were a space tourist, when would you want to y into space? Why? What part of the solar cycle was the Sun in when
you were born?

52
Space Faring: The Radiation Challenge
Answer Key Sunspot Worksheet
Directions: Answer the questions by studying the images of the sun.
Image Credit: NASA Solar and Heliospheric Observatory (SOHO).
(1) Observe the two images of the sun. Describe how the images dier.
e image on the left has many more sunspots than the image on the right. Some of the sunspots are huge while
others are small. ere are no sunspots on the right image.
(2) How many sunspots can you count in the left image?
there are approximately 20 individual spots and 3 or 4 very large clusters of sunspots
(3) How many sunspots are in the right image?
none
(4) In which picture does the sun seem more active? Why?
e left image – there are more sunspots on the sun.
(5) Which solar condition would you predict is better for reducing Galactic Cosmic Radiation exposure to astronauts during long
duration space travel?
For better shielding from Galactic Cosmic Radiation (GCR), the image on the left. A large number of sunspots cor-
responds to more solar activity; because the sun is able to better shield the solar system from harmful GCR during active
periods, space travel during periods of more solar activity might be better to reduce GCR exposure. However, coronal
mass ejections (CME) will be more common, and will pose radiation risks to astronauts. Traveling during years when the
Sun’s activity is similar to the image on the right would help space explorers avoid CME associated with solar maximum.

53
Space Faring: The Radiation Challenge
Answer Key Space Weather Forecasting
Directions: Answer the following questions by using your graph of sun spot data and the sunspot worksheet.
(1) In what year did the most number of sunspots occur?
1949
(2) In what year did the least number of sunspots occur?
1954
(3) On average, how many years are between the peak sunspot activity?
(is period of time is known as the solar cycle).
11 years
(4) Does the sun vary in its activity? Explain.
yes-changes in solar activity are caused by changes in its magnetic eld
(5) Where might the left image from page 1 of the worksheet be located on this graph? Mark the position the graph with a green “O”.
Students could put a green “O” at a solar maximum, or a year of high sunspots, such as in 2001, 2000, 1990, 1989, 1981, 1980,
1970, 1969, etc.
(6) Where might the right image from page 1 of the worksheet be located on this graph? Mark the position on the graph with a
red “X.”
Students could put a red “X” at a solar minimum, or a year of low sunspots, such as in 2006, 1996, 1986, 1976, 1964, etc.
(7) Approximately what year will be the next solar maximum?
2011
Will this be a good travel time for astronauts? Answers will vary Why or why not?
A large number of sunspots corresponds to more solar activity. Because the sun is able to better shield the solar system from
harmful GCR during highly active periods, space travel during solar maximum might be better. Astronauts would potentially be
exposed to less GCR radiation, but will likely be exposed to the radiation dangers associated with CME and solar ares, events that
are common during solar maximum.
(8) Approximately what year will be the next solar minimum?
2017
Will this be a good travel time for astronauts? Answers will vary Why or why not?
Few to no sunspots corresponds to little solar activity. Because the sun is less able to shield the solar system from harmful GCR
during less active periods, space travel for astronauts during solar minimum might be more dangerous because they could
potentially be exposed to much more harmful GCR. However there will be less CMEs and solar ares, so the particle radiation
coming from the Sun will be less.
(9) If you were a space tourist, when would you want to y into space? Why? What part of the solar cycle was the Sun in when
you were born?
Student answers will vary – but presumably students would want to travel during periods of low radiation. Students will refer
to their chart to determine solar activity during the year they were born.

54
Space Faring: The Radiation Challenge
Name: _____________________________________ Date: ________________________
Plotting Sunspots on a Graph Worksheet
Sunspots Per Year
Number of Sunspots (average)
200
180
160
140
120
100
80
60
40
20
0
1940 1945 1950 1955 1960 1965 1970 1975 1980 1985 1990 1995 2000 2005 2010
Year

55
Space Faring: The Radiation Challenge
Answer Key Plotting Sunspots on a Graph Worksheet
Sunspots Per Year
Number of Sunspots (average)
200
180
160
140
120
100
80
60
40
20
0
1940 1945 1950 1955 1960 1965 1970 1975 1980 1985 1990 1995 2000 2005 2010
Year

56
Space Faring: The Radiation Challenge
Applications to Life on Earth: Radiation as a Tool
Now that we have an understanding of radiation, its biological eects, and radiation countermea-
sures, it is important to learn about the benecial uses of radiation. In this section, we will discuss
examples of how ionizing radiation is used at clinics and hospitals to diagnose disease and injury,
and summarize several radiation and radioactive isotope applications.
The Discovery of X-rays
Wilhelm Conrad Röntgen is chiey associated with his discovery of X-rays. In 1895, Röntgen was
carrying out experiments with a cathode ray electron generator (a sealed glass vacuum tube). He
shielded the glowing tube with thick cardboard and was surprised to notice that sensitized paper at
some distance from the tube would still glow – evidently as a result of radiation from the generator.
Röntgen placed his hand between the generator and the coated paper on the wall and was astonished
to observe that the shadow of the bones in his hand had projected on the paper as well! He repeated
this experiment and created a “röntgenogram” of his wife’s hand – the rst ever X-ray image on lm.
For this work, Röntgen was awarded the rst Nobel Prize in Physics in 1901. To this day, radiographs
(X-ray images of a patient’s body) are essential tools in the treatment of disease and injury.
Fluoroscopy
For certain kinds of health conditions, simple radiographs may not be sucient. When
real time observation or medical interventions are required, uoroscopy is commonly used.
Although it exposes a patient to a much higher dose of radiation than a conventional X-ray,
uoroscopy allows a doctor to observe an X-ray image of a patient’s body in real time. is tech-
nique enables doctors to observe surgical procedures like an angioplasty, heart by-pass grafting,
and coronary angiography (an X-ray examination of chambers, blood vessels, and blood ow in
the heart). It also allows for real-time study of gastrointestinal processes.
CT Scanners
Another technique that is based on X-rays technology is computed axial tomography, also
known as CT or CAT Scan. Interestingly, the data imaging techniques previously used on the
spacecraft Mariner 4, which ew by Mars in 1964, eventually lead to medical applications
in CAT scans, diagnostic radiography, brain and cardiac angiography and ultrasound tech-
nologies.
54
CT scanners use X-ray equipment to gather X-ray images from dierent angles around the body in spirals or slices.
Computers are then used to assemble the images for a three-dimensional visualization of the
patient’s internal anatomy. e dose received during one CT Scan is approximately the same as
2-3 chest x-rays equivalents. e same image processing technology has evolved and is used for
applications like crop forecasting, planetary surface characterization, mapmaking, water evalua-
tion, and disaster management.
Nuclear Medicine
Since the discovery of X-rays, scientists and doctors have worked together to develop tools that
allow for imaging of internal anatomy and soft tissues. In nuclear medicine, doctors a variety
of imaging tools with radioactive substances to image a patient’s internal anatomy and func-
tion. is is accomplished by introducing radioactive elements (radioisotopes) into the body
of a patient by injection, inhalation, ingestion, or topical application. Dierent radioisotopes
then preferentially concentrate in certain organs. For example, radioactive iodine-131 collects
in the thyroid gland (see Figure 5).
55
As each radioisotope decays, it gives o radiation (such as
Figure 1: An early X-ray image.
Figure 2: A uoroscope.
Figure 3: A CAT Scan image of a
human head.
54 ht tp://w w w.jpl.nasa.gov/history/index_beginnings.htm
55 ht tp://w w w.fas.org/irp/imint/docs/rst/Intro/Part2_26d.html

57
Space Faring: The Radiation Challenge
gamma rays), which can be observed by a gamma ray camera or detector. Variations in radiation intensity in the body will activate
lm or a detector array to create an image. Typically, the radioisotopes usually have relatively short half-lives and decay rapidly,
which helps to minimize the exposure to damaging radiation. In general, total doses are very low.
Two examples of high-powered imaging tools in nuclear medicine that use the tomographic approach are the Single Photon Emis-
sion Computed Tomography (SPECT) and Positron Emission Tomography (PET) Scanners. ese instruments are especially suited
to monitoring dynamic processes like cell metabolism or blood ow in the heart and lungs. Both use a gamma ray camera to detect
gamma ray photons emitted from the radioisotopes used in the body. In each slice of Figure 6, PET images reveal changes in blood
ow that are correlated with epilepsy in the right side of a patient’s brain. SPECT technology is commonly used in brain scans but
it can also be used to observe other organs such as the heart.
e image that is acquired with a gamma camera or SPECT is called a
scintigram. Figure 7 and 8 show how SPECT imagery can be useful in visualizing along each axis of the heart and brain to compare
its internal structure and function.
Figure 4: The Siemens Symbia SPECT/CT scanner.
Image Credit: Impact Scan.
Figure 5: In this SPECT scintigram,
the radioisotope has selectively
concentrated at abnormal areas in
the thyroid of a cat.
Figure 6: A PET image of an epilepsy patient.
Figure 7: In this nuclear myocardial perfusion tomogram, the SPECT images
are compared with drawings that are similar in cross sectional view. Image
Credit: Yale School of Medicine.
Figure 8: In this normal brain, SPECT and MRI transverse
images can be used to compare structure and function.
Image Credit: Dr. Robert Kohn.

58
Space Faring: The Radiation Challenge
Magnetic Resonance Imaging
Not all medical imaging tools use X-rays or gamma rays. Magnetic Resonance Imaging
(MRI) scans use low energy radio waves and strong magnetic elds to excite magnetic
resonance in tissue atoms. MRI scans are commonly used to dierentiate subtle dierences
within soft tissue regions of the body (dierences in concentrations of water and fat give
rise to dierent MRI signals in these regions). As in CT scan, all or part of the patient’s
body is placed inside a large cylinder during the MRI. A strong magnetic eld is applied,
which causes some of the molecules in the patient to align themselves along the direction
of the eld. is causes the hydrogen-containing compounds within the body to resonate
at radio-frequency signals, which are picked up by a detector. A computer converts it to an
image, which can be color-coded. In some cases, it is useful to combine MRI imagery with
SPECT scintigrams to compare anatomical structures with their function (see Figure 8).
Radiation Therapy
When surgery alone cannot entirely remove a cancerous tumor, radiation therapy
is sometimes used in conjunction with the surgery. Intraoperative radiation therapy
(IORT) delivers a high dose of radiation to cancerous tumors while they are exposed
during surgery. Other techniques like three-dimensional conformal radiation therapy
(3-D CRT) use radiation only. In 3-D CRT (also known as gamma-knife surgery),
computers with specialized software use the information from CT Scans or MRIs to
create beams of radiation that conform to the shape of a tumor. Once the exact loca-
tion, size, and shape of the tumor is known, the computer instructs the linear accelera-
tor to bombard the tumor with the conformal radiation. is technique is particularly
useful in treating prostate cancer, lung cancer and certain brain tumors. Another
example of conformal radiation therapy is Intensity-Modulated Radiation erapy
(IMRT), which precisely varies the intensity of the radiation beams used during treat-
ment. Greater radiation intensity is directed at larger areas of the tumor, while weaker beams are directed to smaller areas of the
tumor. is helps to reduce the amount of radiation used and limits the amount of radiation exposure to healthy tissue. In some
cases, radiation is also combined with heat in treatments to kill cancer.
Brachytherapy
In each of the previously discussed examples, radiation is delivered from a source exter-
nal to the patient’s body. However, there are internal forms of radiation therapy like
Brachytherapy, which is designed to deliver a high dose radiation from inside the body.
Brachytherapy involves placing a protected source of radiation (such as Iridium-192 or
Cesium-131 that has been encased in tubes, wires, or capsules, see Figure 11) directly
within the tumor or very near to it.
Side Effects of Radiation Therapy
Exposure to radiation can cause negative side eects, ranging from dry mouth, diculty
swallowing, changes in taste, nausea, vomiting, diarrhea, irritated skin, hair loss, chest
tightness, cough, shortness of breath, fatigue, or ear aches. In addition, physiological
complications like bone marrow suppression may result. is can cause anemia, low
white blood cell count, and low platelet count. Secondary malignancies or treatment-
associated cancers can sometimes occur in patients years after radiation therapy. Some
patients experience damage to healthy tissues that leads to cognitive impairment, or the
loss of the ability to remember, learn, and complete certain tasks. As a result, a great deal of research focuses on maximizing the
benets of tumor killing radiation while minimizing its eects on healthy tissue surrounding the tumor. It is important to note
that the location and intensity of radiation exposure aects the nature of negative side eects.
Figure 9: An MRI scanner.
Figure 10: Radiation therapy uses radiation to
treat disease. Image Credit: Mayo Clinic.
Figure 11: Tiny capsules lled with Cesium-131
are implanted in or near a tumor. X-rays emitted
by the cesium kill the cancer cells. Image
Credit: Pacic Northwest National Lab.

59
Space Faring: The Radiation Challenge
Biotechnological and Chemical Uses
ere is a great deal of ongoing biochemical research that uses radiation sources. Much of this work investigates the molecular
mechanisms responsible for biological processes. For example, scientists use high-intensity X-ray beams in crystallography to pro-
duce images of the crystal structures
56
of biochemicals such as the avin-containing monooxygenase seen in Figure 12. By studying
the crystal structure of biochemicals, scientists are able to create step-by-step snapshots of chemicals at dierent stages of catalytic
action. Crystallography is also used to create three-dimensional structures of particular proteins with the purpose of designing
drugs that interact specically with these proteins. Other researchers use radioactive isotopes in chemistry labs to track the path a
chemical follows during a chemical reaction. To accomplish this, radioactive isotopes are incorporated into reactants, the chemicals
are mixed, and the reaction is carefully monitored over time. is procedure is particularly useful for tracing underground rivers,
following blood supply to a brain tumor, visualizing brain function itself, or the development of an embryo.
Radiometric Dating
Radiometric dating is a technique used to date both physical and biological matter. It is based on knowing the decay rates of natu-
rally occurring isotopes. Radioactive decay is a spontaneous process in which an unstable atom emits particles (electrons or much
heavier alpha particles–helium nuclei) from its nucleus to create a dierent form (an isotope) of the same element. e rate of
decay is expressed in terms of an isotope’s half-life, or the time it takes for one-half of the radioactive isotope in a sample to decay.
Most radioactive isotopes have rapid rates of decay (short half-lives) and lose their radioactivity within a few days or years. Some
isotopes decay much more slowly over millions or billions of years, and serve scientists as “geologic clocks.”
57
Geologists can deter-
mine the age of a geologic formation or fossil by using a mathematical formula in Figure 13.
58
Figure 12: The half-life of naturally occurring radioactive substances in a sample
can be used to determine the age of the sample. Image Credit: USGS.
Figure 13: Radiation can be used to learn about the shape of
enzymes. Image Credit: Brookhaven National Lab.
56 ht tp://w w w.bnl.gov/bnlweb/pubaf/pr/PR_display.asp?prID=06-76
57 ht tp://pubs.usgs.gov/gip/geotime/radiometric.html
58 ht tp://pubs.usgs.gov/gip/geotime/radiometric.html

60
Space Faring: The Radiation Challenge
Consumer Products
Many common consumer products are manufactured with, or naturally contain, radioactive material. Examples include smoke
detectors, watches, clocks, ceramics, glass, camera lenses, fertilizers, and gas lantern mantles. Foods that have a low sodium salt
substitute may contain potassium-40. In the 1920s, some products were sold as radium-containing “cure-alls!”
Power Sources
Heat produced from the decay of radioactive substances can be used to generate electricity by means of radioisotope thermoelectric
generators (RTGs). e Pioneer, Viking, Voyager, Galileo, Ulysses, and Cassini (Figure 14)
59
spacecrafts all used this technology.
60
On larger scales, electrical energy can also be produced through ssion of radioactive materials like Uranium 238.
Sterilization and Food Irradiation
In biology or tissue culture laboratories, UV radiation is an essential part of everyday operations in facilities that require sterile
conditions during cell plating, tissue handling, or specimen transfer. Prior to sensitive operations, UV radiation is used to sterilize
surfaces to ensure clean working conditions before the operations begin. Notice the bright blue light in the picture in Figure 15.
It is a UV light inside a laminar ow hood. When it is turned on, the internal work volume of the hood is being sterilized.
One method of preserving fresh or packaged food is to expose it to ionizing radiation, which is a process known as cold pasteuri-
zation. is process kills any microbes that could cause spoilage or disease to the consumer. Food sterilization by radiation is the
most studied food preservation process and has been shown to be safe and reliable.
Figure 14: The Cassini spacecraft.
Figure 15: UV lights inside a laminar ow hood at NASA Ames.
59 ht tp://solarsystem.nasa.gov/multimedia/gallery.cfm?Category=Spacecraft&Page=15
60 ht tp://nuclear.energy.gov/space/neSpace2a.html

61
Space Faring: The Radiation Challenge
Glossary
Acute exposure is short-term, high-level exposure to radiation. e eects of acute radiation exposure become more severe as the
exposure increases. Health eects from acute exposure to radiation usually appear quickly. e physical response is called radiation
sickness, or radiation poisoning.
e Central Nervous System (CNS) is the brain and the spinal cord. You use this system to think and to take action. e CNS
helps to coordinate muscle and organ activity, and monitor input from your senses.
Chronic exposure is long-term, low-level exposure to radiation. Higher levels of radiation exposure make these health eects more
likely to occur, but do not inuence the type or severity of the eect. Examples of health eects from chronic radiation damage
include cancer, leukemia, and genetic changes.
Chromosomes are the forms in which genetic information, DNA (deoxyribonucleic acid), are packaged in our cells. Human cells
contain 23 pairs of chromosomes. Each chromosome contains a single long thread of DNA, wrapped around proteins that help
keep the DNA organized within the cell. e blueprint for life (as we know it) is contained within DNA.
Coronal Mass Ejections (CME) are explosions that occur on the surface of the Sun. ese eruptions release massive amounts of
energy out into space in the form of X-rays, gamma rays, and streams of protons and electrons called solar particle events. CME
can be very harmful to space explorers.
DNA (deoxyribonucleic acid) is the molecule that encodes genetic information in cells. DNA consists of two strands of alternat-
ing phosphate and deoxyribose sugar molecules zipped together by pairs of nucleotide bases. e four nucleotides in DNA contain
the bases adenine (A), guanine (G), cytosine (C), and thymine (T). In nature, base pairs form only between A and T and between
G and C; thus the base sequence of each single strand can be deduced from that of its partner.
Galactic Cosmic Radiation (GCR) are charged particles moving at nearly the speed of light. ey can cause damage as they pass
through matter and can pass practically unimpeded through a typical spacecraft or the skin of an astronaut. GCR consists mostly
of protons (nuclei of hydrogen atoms), some alpha particles (helium nuclei), and lesser amounts of nuclei of carbon, nitrogen, oxy-
gen, and heavier atoms. During solar maximum, GCR passing through our solar system is deected (lessened) because changes in
the Sun’s magnetic eld due to solar ares and coronal mass ejections. GCR can be very harmful to space explorers.
Hematopoietic syndrome refers to the symptoms caused by the eects of radiation on blood producing organs (spleen, lymph
nodes, and bone marrow). Damage to these organs can cause a shortage of white blood cells, red blood cells, and platelets, which
can lead to anemia, bleeding, fatigue, weakness, and infections.
Prodromic syndrome refers to the initial symptoms (nausea, vomiting, and diarrhea) that indicate radiation poisoning.
Solar Cycle is the 11-year cycle of the Sun. During this period, the Sun varies in activity, producing large numbers of sunspots at
solar maximum, and few during solar minimum. Solar maximum returns approximately every 11 years.
Solar Maximum is the period of greatest solar activity during the Sun’s 11-year solar cycle. During solar maximum, the Sun is
highly active and has many sunspots. Its magnetic eld is more able to eectively shield the inner solar system from galactic cosmic
radiation, but numerous solar ares and coronal mass ejections with harmful particle radiation are common.
Solar Minimum is the period of least solar activity during the Sun’s 11-year solar cycle. During solar minimum, the Sun is rela-
tively inactive and has few sunspots. Its magnetic eld is unable to eectively shield the inner solar system from galactic cosmic
radiation. Solar ares and coronal mass ejections are rare or absent.

Space Faring:
The Radiation Challenge
EDUCATOR REPLY CARD
To achieve America’s goals in Educational Excellence, it is NASA’s mission to develop
supplementary instructional materials and curricula in science, mathematics, geogra-
phy, and technology. NASA seeks to involve the educational community in the
development and improvement of these materials. Your evaluation and suggestions are
vital to continually improving NASA educational materials.
Please take a moment to respond to the statements and questions below.
You can submit your response through the Internet or by mail. Send your
reply to the following Internet address:
https://neeis.gsfc.nasa.gov/JDbGenie/vol1/htdocs/edcats/rhsf_edu_reply_card.html
You will then be asked to enter your data at the appropriate prompt.
Otherwise, please return the reply card by mail. Thank you.
1. With what grades did you use the educator guide?
Number of Teachers/Faculty:
K-4 5-8 9-12 Community College
College/University - Undergraduate Graduate
Number of Students:
K-4 5-8 9-12 Community College
College/University - Undergraduate Graduate
Number of Others:
Administrators/Staff Parents Professional Groups
General Public Civic Groups Other
2. What is your home 5- or 9-digit zip code? –
3. This is a valuable educator guide?
Strongly Agree
Agree
Neutral
Disagree
Strongly Disagree
4. The information provided in the product is relevant to my role in education.
Strongly Agree
Agree
Neutral
Disagree
Strongly Disagree
5. How would you rate the effectiveness of the product in teaching the intended
standards.
Excellent
Good
Average
Poor
Very Poor
6. How did you use this educator guide?
Background Information
Critical Thinking Tasks
Demonstrate NASA Materials
Demonstration
Group Discussions
Hands-On Activities
Integration Into Existing Curricula
Interdisciplinary Activity
Lecture
Science and Mathematics
Team Activities Standards Integration
Other: Please specify:
7. Where did you learn about this educator guide?
NASA Educator Resource Center
NASA Central Operation of Resources for Educators (CORE)
Institution/School System
Fellow Educator
Workshop/Conference
Other: Please specify:
8. What features of this educator guide did you find particularly
helpful?
9. How can we make this educator guide more effective for you?
10. Additional comments:
Today’s Date:

Please Place
Stamp Here
Post Office
Will Not Deliver
Without Proper
Postage
MARSHALL SPACE FLIGHT CENTER
ACADEMIC AFFAIRS OFFICE
HS30
C/O INFORMAL EDUCATION
HUNTSVILLE, AL 35812
!2054600012!
Fold along line and tape closed.
National Aeronautics and Space Administration
George C. Marshall Space Flight Center
Huntsville, AL 35812
w w w.nasa.gov/marshall
w w w.nasa.gov
8-383128
